
Paediatric patients represent 5–15% of emergency medical services (EMS) transports in the US, yet true paediatric emergencies are rare. Management of these cases remains a common area of discomfort for pre-hospital providers. Previous studies have shown that simulation-based medical education is a useful tool to enhance patient safety in paediatrics. Simulation is an ideal modality to evaluate cognitive, technical and behavioural skills in low frequency, high-stakes events for healthcare providers. We hypothesize that using a deliberate practice model with simulation through a 6-month longitudinal curriculum will improve performance among pre-hospital providers treating paediatric seizure patients.
A prospective observational education study design of a 6-month longitudinal simulation curriculum was executed. The performance of each two-member fire-based crew was analysed during three separate simulation events. The in situ simulations were video recorded and conducted within an ambulance. Performance was reviewed and scored by three reviewers. A comparison analysis was reported.
Thirty-nine pre-hospital providers completed at least some portion of the curriculum. There was an improvement in provider reported self-efficacy scores across all questions, as well as improvement in pre- and post-test knowledge scores. While the total number of critical actions completed did not vary significantly between simulations, there was improvement in several action items including end-tidal carbon dioxide use, application of oxygen, checking of medication dosage and administration of correct benzodiazepine dose.
A simulation-based curriculum on the management of paediatric seizure for EMS providers improved self-efficacy, knowledge and performance of various critical actions in simulated settings.
What this study adds
Paediatric patients represent 5–15% of emergency medical services (EMS) transports in the US, yet true paediatric emergencies are rare [1]. Management of paediatric patients remains a common area of discomfort for pre-hospital providers. The needs of children differ from adults treated in the pre-hospital setting. Pre-hospital care providers must have appropriate equipment, training, and safe and effective protocols to treat children [2]. The importance of identifying effective paediatric education and skills retention training has been highlighted repeatedly in the literature published by the National Association of Emergency Medical Services Physicians (NAEMSP), the Emergency Medical Services for Children (EMS-C) as well as the Pediatric Emergency Care and Applied Research Network (PECARN) [1,2].
In 2010, PECARN highlighted research priorities for paediatric pre-hospital care including both airway management and seizures. They also highlighted systems level research priorities including out-of-hospital interventions, knowledge and skill deterioration and training effectiveness [2]. PECARN revisited research priorities in 2015, again stressing airway management, seizures, training and competency as top priorities, along with the addition of vascular access research [1]. Since this publication, multiple studies have attempted to address the individual priorities utilizing simulation as the primary study focus. Shah et al. demonstrated dosing errors for paediatric seizure patients receiving midazolam occurred in 49% of cases [3]. Even with accurate weights the medication was under-dosed in 87% of those patients. Hansen et al. identified that pre-hospital providers have paediatric specific gaps in case exposure, competency and knowledge, assessment and decision-making, and critical thinking and proficiency [4].
Simulation is an important educational tool in building, improving and maintaining necessary skills among pre-hospital providers [5]. Additionally, simulation-based medical education (SBME) is a useful tool to enhance patient safety in paediatrics [6]. Simulation of paediatric emergencies under reasonably realistic field conditions provides an alternative to direct field observation [7]. Previous studies demonstrated that paramedic student error rates decreased when simulation was used to instruct specific components [8]. They have also shown that replacing parts of clinical requirements with simulation is equal to or even more effective than an equivalent clinical experience [8]. The deliberate practice method of simulation emphasizes the immediate application of learning points during successive simulations. In this scenario, learners receive feedback through a debriefing session after an initial simulation. Following the debrief, the learners complete a second simulation session with similar learning objectives. This succession allows learners to cement the knowledge gained during feedback. Deliberate practice provides more effective learning by offering participants an opportunity to immediately implement and demonstrate the insight provided through the debriefing session [6]. Repeated simulation exercises carried out over time improve the ability to recall knowledge and increase the level of experience leading to improved patient care [3,9].
Seizures are a common reason EMS is called for paediatric patients [3]. Management of paediatric seizures can be complex requiring multiple seldom used skills, including paediatric IV placement, weight-based medication dosing and advanced airway management. The complexity of seizure management coupled with its relative frequency in the pre-hospital setting make it an ideal educational opportunity for simulation-based education. We hypothesize that using a deliberate practice model with simulation through a 6-month longitudinal curriculum will improve performance among pre-hospital providers treating paediatric seizure patients. Secondarily, we hypothesize that provider self-efficacy and knowledge in caring for paediatric seizure patients will improve over the same time frame.
A prospective observational education study design of a 6-month longitudinal simulation curriculum was conducted with a convenience sample of 39 subjects (Figure 1). This study was approved by the IRB at Indiana University. Self-efficacy surveys were completed by each participant prior to each of the simulation events. A final self-efficacy survey was completed 1 month after the final simulation. Each participant also completed a knowledge-based questionnaire prior to the first simulation and following the final simulation at the 6- or 8-month mark depending on when the crews completed their curriculum. Each simulation event was video recorded for later review and critical action scoring. A debriefing occurred after each simulation scenario to evaluate stated objectives. The simulation events employed a deliberate practice model of simulation education wherein a simulation was conducted. The crew then participated in a formal debrief with directed feedback and education from paediatric experts. Following the debrief the crew participated in a second simulation with the same stated goals and critical actions. This process allowed learners an opportunity to apply concepts discussed during debriefing (see Figure 2). The debriefing after each simulation scenario focused on the stated objectives. The study was initially designed to occur over a 7-month timeline. However, due to the COVID pandemic, the timeline was adjusted for safety concerns. Four of the 12 crews completed the third simulation event at 6 months, while the remaining eight crews completed the third simulation event at 8 months. All participants received the final self-efficacy survey 9 months after their initial simulation session.

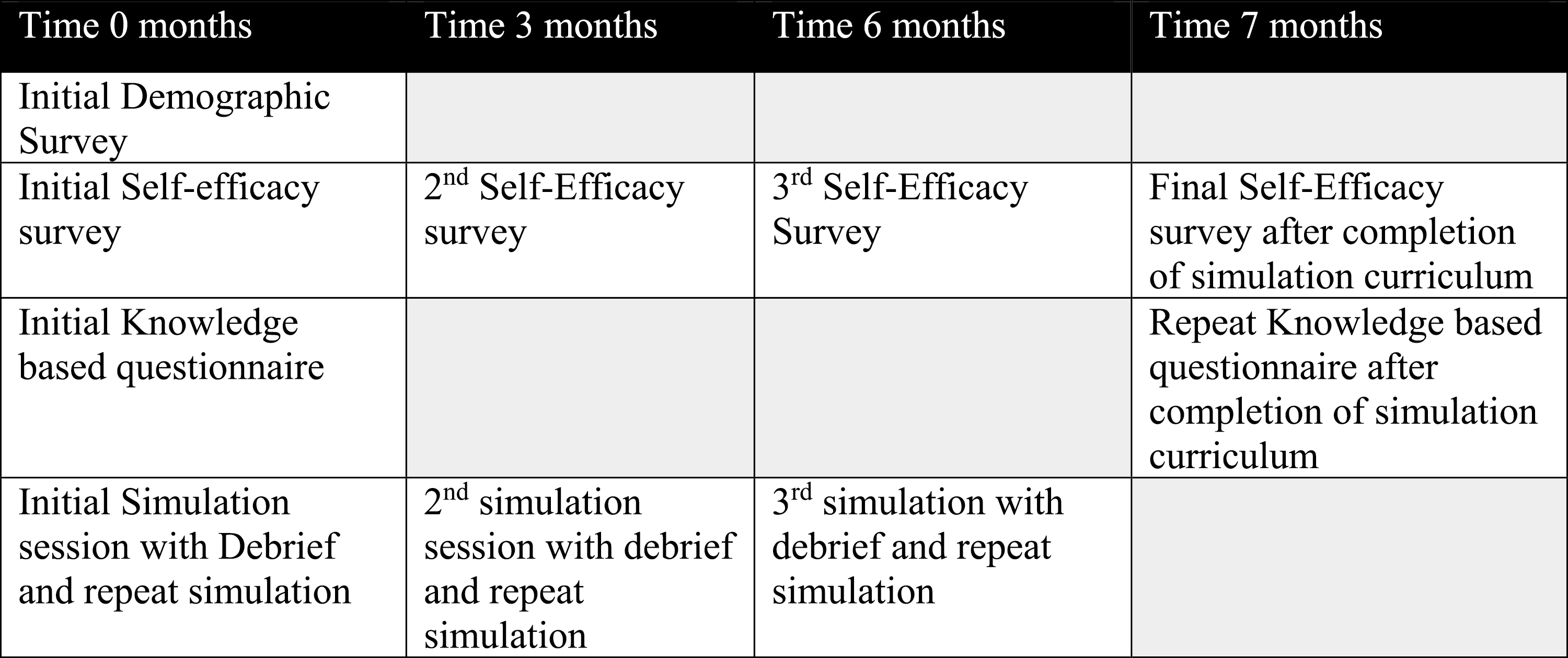
Curriculum design.

Pre-hospital personnel undergoing formative training on paediatric seizure management.
Paediatric status epilepticus was the primary diagnosis for all of the scenarios completed over the study period. The first scenario was a patient with a history of seizures having breakthrough status epilepticus. In the 3-month simulation, the scenario was a patient with a febrile status epilepticus. For the final scenario, the patient was hypoglycaemic resulting in status epilepticus. The curriculum was designed to have a graded level of difficulty with the same underlying diagnosis to challenge skills of the participants as well as preventing flippant management from the previous simulation cases.
Status epilepticus was chosen as the primary pathology because it offered the opportunity to evaluate multiple cognitive and procedural skills of the participants including paediatric assessment, vital sign recognition, weight-based dosing, medication administration, airway management and paediatric bag valve mask performance.
The simulation events were conducted over an 8-month period and included a total of nine events. Each simulation event (0, 3, and 6/8 months) included three simulation days to capture all three EMS shifts (A, B, C). Each crew was taken out of service for 1 hour at a time to participate in the simulation training. The demographics, self-efficacy and pre-test surveys were collected via RedCap and completed prior to the simulations starting. The emergency medical technician (EMT)-B (basic) and EMT-Ps (paramedics) who participated also completed a 10-question multiple choice knowledge-based questionnaire on paediatrics and seizure management prior to the first simulation.
Each of our simulation events began with orientation of the participants to the simulation mannequin to address functionality and demonstrate capabilities. A Laerdal Sim Junior™ was used for the scenarios. Crews were also provided with a mock-up version of the resuscitation bags available on their ambulances to use during the simulations.
After orientation the participants completed the first of two simulation scenarios. Upon completion of the first scenario, a debriefing session was led by a member of the training staff to discuss the case providing feedback on the team performance. Participants were asked to reflect on their actions and consider changes to be used in future simulations and in actual patient care. Following the debrief, an additional deliberate practice simulation scenario was completed. The learning objectives and critical actions were unchanged between the first and second scenario, however, the size and age of the child differed as did certain historical and case features. A debriefing after the second scenario completed the simulation event.
The complete training staff included three board certified EMS physicians, one EMS fellow, two simulation fellows and three Emergency medicine residents. Both the EMS fellow and two of the EMS physicians were also trained in Paediatrics and practice Paediatric Emergency Medicine. There were 3–4 members of the training staff at each simulation event. The debriefings were conducted in a team fashion amongst the training staff.
Three different types of surveys were utilized to provide context to the simulation performance. The first survey collected demographic information including age, gender, years of experience, level of training and ongoing paediatric education (Appendix 1). The second survey was a self-efficacy survey designed to explore provider confidence in both caring for children and participating in simulation education. The self-efficacy questionnaire was modified from a tool created by Craven et al. and utilized a visual analogue scale measuring confidence in specific skills and knowledge [10]. The self-efficacy surveys were collected at four distinct times: prior to the first simulation, prior to the 3- and 6/8-month simulations, and 9 months from the initial simulation. The third survey, a 10-question knowledge-based questionnaire on paediatric care and seizure management was given to EMTs prior to the first simulation event and again at the conclusion of the simulation curriculum (Appendix 2).
An unvalidated critical action checklist (Appendix 3) was created by the co-authors based on the current best practices of paediatric status epilepticus according to local EMS protocol, and evidence-based practice [11,12]. The checklist was modified during pilot testing and after initial scenario completion taking into account the nature of simulation education as well as the EMS work environment which requires multiple tasks to be managed at once. This process rendered some of the critical action items difficult to score. A modification to two items allowed for inclusion of different methods of performing the same task, for example, considering multiple methods to reposition the airway instead of only a jaw-thrust manoeuvre as initially stated on the checklist.
The participants are all employed by a single township fire department. The fire department serves a population of ~140,000 and responds to approximately 16,000 calls per year. There are four ambulances per 24-hour shift staffed by an EMT and paramedic or two paramedics. Due to the complexity of scheduling, our intent was to touch as many providers as possible without relying on them being with the same partner for each simulation event.
The simulations were conducted in situ using a fully functioning reserve type 3 ambulance owned by the fire department. The ambulance was temporarily modified for the purpose of this study with a temporary camera mount for video review purposes.
The simulations were video recorded and graded for completion of critical actions (Appendix 3) by three physician reviewers with expertise in EMS and paediatric emergency medicine. The three physician reviewers were trained on completion of the critical action checklist by one of the study co-primary investigators.
While simulation pre-survey notes the video would be used for debriefing as well, this was not feasible while also performing the simulation in an ambulance, therefore video was only used for grading the critical actions. Two GoPro cameras (one mounted above the airway seat and one worn as a chest strap on one of the participants) were used to video record each simulation.
Demographics and EMS completed checklist items were summarized using frequencies and percentages. EMS self-assessment surveys and knowledge scores were summarized using mean and standard deviation. Fisher’s Exact and Wilcoxon Rank-Sum tests were utilized for statistical analysis. A kappa statistic was also calculated between the three physician reviewers. All statistical analyses were completed using SAS Version 9.4.
Thirty-nine participants completed at least some portion of the curriculum. Fifteen completed one simulation event. Fifteen completed two simulation events and nine completed the entire curriculum. The majority of the participants were EMT-paramedics (76%) with a male predominance (63%). The majority were experienced pre-hospital providers with only two (5%) having less than 1 year of experience (Table 1). Thirty (76%) participants were paediatric advanced life support (PALS) certified, while five of the participants reported that they had not had any formal paediatric training in the prior 2 years. Most, (32/39, 94%) participants reported interest in integration of simulation into training prior to the first simulation event (Table 2).

| Age | |
|---|---|
| 18–23 | 3 (7.9) |
| 24–29 | 9 (23.7) |
| 30–35 | 12 (31.6) |
| 36 or above | 14 (36.8) |
| Gender | |
| Male | 24 (63.16) |
| Female | 13 (34.21) |
| Prefer not to answer | 1 (2.6) |
| Training level | |
| EMT-basic | 9 (23.7) |
| EMT-paramedic | 29 (76.3) |
| Years of experience | |
| 0–1 | 2 (5.3) |
| 2–5 | 12 (31.6) |
| 6–10 | 13 (34.2) |
| 10+ | 11 (29.0) |
| Paediatric patients monthly, mean (Std) | 4.2 (5.1) |

| Training | |
| Paediatric advanced life support (PALS) | 30 (76.9) |
| Advanced paediatric life support (APLS) | 2 (5.1) |
| Paediatric education for pre-hospital providers (PEPP) | 6 (15.4) |
| Emergency paediatric care (NAEMT) | 2 (5.1) |
| Paediatric emergency course/conference | 0 (0.0) |
| Other paediatric course | 9 (23.1) |
| None | 5 (12.8) |
| Additional information | |
| Previous simulation participation | 7 (18.9) |
| Simulation integration interest | 32 (94.1) |
| Belief that simulation is a valuable tool | 34 (91.9) |
All participants completed self-efficacy surveys prior to simulation. Table 3 shows the values on a visual analogue scale 1–100 for each question on the assessment. There is an increasing trend of confidence between each simulation session for each question. There is significant improvement across all questions comparing pre- and post-simulation self-efficacy scores.

| Pre-simulation | 3 months | 6 months | 7 months | P-Value* | |
|---|---|---|---|---|---|
| Knowledge base when caring for paediatric patients. | 64.7 (18.6) | 66.9 (20.6) | 71.4 (16.9) | 81.8 (11.4) | 0.0007 |
| Patient assessment skills in caring for paediatric patients. | 70.2 (17.6) | 69.8 (20.4) | 75.5 (15.9) | 82.3 (13.2) | 0.0291 |
| Recognizing normal vital signs for age. | 68.0 (14.6) | 67.8 (13.0) | 76.8 (13.0) | 82.2 (13.3) | 0.0005 |
| Caring for paediatric patients in general. | 71.7 (17.3) | 71.2 (20.5) | 71.2 (18.0) | 85.5 (12.1) | 0.0036 |
| Recognizing paediatric patients with seizure. | 75.4 (12.7) | 75.8 (13.5) | 82.3 (13.2) | 88.1 (13.2) | 0.0004 |
| Treating paediatric patients with seizure. | 72.6 (16.2) | 75.2 (17.9) | 80.9 (12.8) | 87.7 (13.6) | 0.0005 |
| Assessing a child’s respiratory status. | 73.4 (15.2) | 74.0 (17.2) | 78.2 (14.4) | 86.3 (12.5) | 0.0029 |
| Recognizing paediatric patients in respiratory distress. | 75.3 (13.8) | 74.5 (17.9) | 83.3 (14.0) | 85.7 (13.3) | 0.0069 |
| Providing bag valve mask ventilation to paediatric patients. | 82.5 (14.9) | 82.4 (14.8) | 87.4 (11.9) | 92.3 (9.0) | 0.0181 |
| Technical skills when caring for paediatric patients. | 70.5 (20.4) | 74.9 (15.3) | 76.4 (16.7) | 85.5 (12.2) | 0.0070 |
| Choosing age- and size-appropriate equipment. | 74.2 (16.1) | 74.3 (20.5) | 78.3 (14.1) | 85.9 (13.5) | 0.0109 |
| Knowing intraosseous technique | 66.0 (27.6) | 82..4 (8.4) | 77.8 (22.0) | 88.3 (13.1) | 0.0006 |
| Calculating paediatric medication dosing. | 53.9 (29.5) | 69.2 (24.7) | 70.6 (25.4) | 83.6 (15.3) | <0.0001 |
| Administering IN/IM/IV medications. | 61.2 (31.7) | 82.2 (13.7) | 77.2 (21.9) | 89.9 (12.9) | <0.0001 |
*Estimated using Wilcoxon test.
Pre- and post-knowledge-based testing improved significantly in both the EMT-B and EMT-P groups. The EMT-B group improved from an average of 66.7% correct on the pre-test to 80% on the post-test. The EMT-P group improved from 79.6% on the pre-test to 85% correct on the post-test. The scores of the pre- and post-knowledge tests significantly improved (p = 0.01) for the entire cohort.
A kappa statistic was calculated between the three physician reviewers and was found to be 0.52 indicating moderate agreement. Evaluating the completed critical actions, there was not a statistically significant change in the total number of critical actions completed between the simulation events. There was a significant improvement in initial application of oxygen (O2), use of end-tidal carbon dioxide (ETCO2 ), confirmation of appropriate weight-based dosing, and administration of the first correct dose of midazolam per protocol (Table 4). Verbalizing respiratory depression, checking bedside glucose, determining weight for weight-based dosing and reassessment of the patient after medication administration were critical actions that were noted to not have statistically significant differences between the simulation events.

| Completed actions | Pre-simulation | 3 months | 7 months | P-Value* |
|---|---|---|---|---|
| Airway/breathing assessment (checks mouth, observes chest rise) | 87 (81.3) | 57 (93.4) | 38 (74.5) | 0.0171 |
| Circulation assessment (checks BOTH pulse and capillary refill) | 49 (46.2) | 45 (76.3) | 21 (41.2) | 0.0001 |
| Neurological assessment (AVPU score) a. Assess pupil response b. Assess response to painful stimuli |
39 (36.8) | 33 (54.1) | 17 (33.3) | 0.0437 |
| Verbalize respiratory depression | 92 (87.6) | 54 (90.0) | 45 (88.2) | 0.9249 |
| Apply supplemental oxygen appropriately (NC, NRB) within 30 seconds | 97 (89.7) | 61 (100.0) | 49 (96.1) | 0.0118 |
| Perform chin lift, jaw-thrust manoeuvre using appropriate technique | 57 (57.0) | 33 (57.9) | 26 (50.9) | 0.7478 |
| Perform BVM ventilation using appropriate technique | 84 (77.8) | 51 (85.0) | 43 (84.3) | 0.4624 |
| Perform BVM using appropriate rate (~20 per minute) | 96 (90.6) | 51 (85.0) | 35 (70.0) | 0.0055 |
| Utilize ETCO2 during BVM ventilation | 74 (69.2) | 48 (80.0) | 41 (82.0) | 0.1459 |
| Verbalize seizure onset | 96 (95.1) | 60 (100.0) | 51 (100.0) | 0.0828 |
| Check bedside glucose | 98 (92.5) | 58 (96.7) | 49 (98.0) | 0.3364 |
| Determine weight for weight-based dosing | 103 (98.1) | 61 (100.0) | 51 (100.0) | 0.7267 |
| Confirmation of appropriate dose based on weight using paediatric medication cards | 88 (85.4) | 56 (96.6) | 49 (96.1) | 0.0258 |
| Two-person verification of medication used | 55 (52.9) | 28(45.9) | 25 (49.0) | 0.6765 |
| Administer first correct dose of midazolam per protocol *IV/IM/IN Midazolam/ (0.1 mg/kg) |
87 (80.6) | 59 (100.0) | 36 (70.6) | <0.0001 |
| Administer 2nd dose of midazolam after 5 minutes Max 2 IV, Max 1 IN, IM |
73 (71.6) | 44 (83.0) | 26 (50.9) | 0.0017 |
| Verbalize diagnosis of status epilepticus | 20 (19.4) | 58 (96.7) | 33 (64.7) | <0.0001 |
| Place IV/IO | 84 (80.0) | 52 (85.3) | 43 (84.3) | 0.7150 |
| Protocols available and/or verbalizes use | 69 (70.4) | 51 (89.47) | 48 (96.0) | <0.0001 |
| Reassessment of patient after medication administration | 101 (96.2) | 61 (100.0) | 51 (100.0) | 0.1887 |
| Total number of observations per event | 103 | 61 | 51 |
*Estimated using Fisher’s Exact test.
We defined a drug dosing error as >20% difference compared to the weight-appropriate dose based on previous literature [13]. Based on this definition we had 8 dosing errors (12%) during the first simulation, 5 errors in the second simulation (8%) and 14 dosing errors in the third simulation (21%). There were 2 dosing errors in excess of the weight-appropriate dosing across our 3 simulation events totalling 68 individual simulations. There was a local protocol change prior to the third simulation event that increased the IM/IN dosing of midazolam to 0.2 mg/kg while the IV dosage remained at 0.1 mg/kg. This was the cause of some of the medication dosing errors in the third simulation event. When factoring for the protocol change there were 4 dosing errors (2%) and all of them resulted in underdosing. Most dosing errors occurred as a result of a mistake in one or more of the four following areas: (1) incorrect patient weight assessment; (2) use of the incorrect per kilogram dosing of midazolam; (3) incorrect calculation of dose in mg; or (4) incorrect volumetric conversion of medication dosage. The use of incorrect per kilogram dosing was frequently related to a failure to remember differences in per kilogram dosing among the different routes of administration. Of note, medication double checks between providers were also often incompletely performed. For example, the provider calculating and drawing up the medication might show their partner the syringe and volumetric calculation but not show them the medication vial or report the per kilogram dosing they were using. These omissions in the medication double checks also contributed to overall dosing errors.
This study demonstrates that the use of simulation with a deliberate practice approach for the training of pre-hospital providers is an effective methodology to improve confidence, knowledge and performance of some critical actions in the resuscitation of paediatric seizure patients. Self-efficacy scores, paediatric knowledge scores, drug dosing calculations and airway management during simulation scenarios improved significantly during this study. This curriculum provides an effective approach to ensure pre-hospital providers remain proficient in several infrequently used but critical skills.
Provider self-efficacy improved in paediatric airway management, specifically with assessment of paediatric airway, recognition of respiratory distress in a paediatric patient and providing BVM to a paediatric patient. Participants reported to the training staff during the simulations that they would like more trainings involving simulation and felt more comfortable with paediatrics after completing the scenarios and debriefing with our training staff. This is supported in the self-efficacy data as there was improvement in self-efficacy after each simulation event. There was also improvement in their actions as the curriculum progressed with increased use of EtCO2, improvement in BVM technique amongst the providers, and delivery of appropriate ventilation rate to the simulated paediatric patient.
Despite the improvement in self-efficacy and knowledge, there was not a statistically significant improvement in the composite score of completed critical actions. The overall number of completed critical actions remained essentially the same, but some of the more clinically relevant aspects of management did demonstrate improvement. Confirmation of medication dosing and administration of the first correct dose of benzodiazepine both reached statistical significance.
Utilization of ETCO2, and application of O2 were other findings from the critical actions that demonstrated improvement throughout the curriculum. These airway interventions may have significant impact on patient outcomes as they minimize hypoxia and allow for earlier recognition of respiratory depression in the child with status epilepticus [14,15].
Several of the critical actions did not reach statistical significance throughout the curriculum because they were completed >90% of the time in all three events. The consistent superior performance in these areas contributed to there being no overall difference in the number of critical actions completed. These items included verbalizing seizure onset, checking bedside glucose, determining weight for weight-based dosing and reassessment of the patient after medication administration. Given the importance of these actions in the management of paediatric status epilepticus it was reassuring to the research team that they were consistently performed throughout the curriculum. It was also noted that there was a decrease from the second to third simulation events in several of the critical actions after an initial large improvement from the first to second event.
Route of medication administration was another focus of the critical action list. The majority of providers attempted IV access initially in the first round of simulations. By contrast, IM/IN was the preferred route of administration in all of our 3-month and 6/8-month simulations. This change likely resulted in quicker time for medication administration during the scenarios. As shown in the self-efficacy survey, the training improved providers comfort with medication routes of administration as well as time to medication administration via IM/IN over IV route. This improved comfort also led to increased use of the IM/IN route during scenario performance.
Medication dosing errors have been well documented in the literature previously, and they were noted in our study as well [3,7,13,16]. There were multiple medication dosing errors during the simulations and the errors continued throughout the study despite improved confirmation of appropriate doses between trainings. There was an increase in the practice of 2-person confirmation of medication dosing, yet due to errors in Broselow tape utilization or dosage calculations under pressure during scenarios, medication errors persisted. This finding further highlights the need for easier methods for pre-hospital providers to determine weight in paediatric patients as well as minimize the need for medication dose calculations [17]. Paediatric smartphone apps and laminated drug dosing cards have been developed to help with both of these issues, but more work needs to be done in this area, including additional training and education for EMS personnel. We also suspect there may have been some dosing errors based on the design of the silhouette cut-outs, but this accounted for a small percentage overall.
As part of the curriculum design there was a component of increasing difficulty with regard to simulations as the curriculum progressed. This is seen as a strength of the educational design as it demonstrated to the participants how multiple different causes can lead to the same end diagnosis, in this case status epilepticus. It also showed the importance of factoring in all these features when determining appropriate treatment for the patient. Ultimately, this process provided a platform for additional discussion and education during the debriefs. In most cases the debrief confirmed the participants management decision, but in some cases provided clarification and improvement in underlying knowledge of appropriate treatment and management.
Future aims include utilizing the recorded video footage to conduct a subgroup analysis using team dynamics tools to assess communication and teamwork aspects amongst EMS crews. Based on the results of this study, the investigators plan to expand this curriculum to other EMS agencies with the goal of continuing to improve paediatric pre-hospital medical care.
There were several limitations of this study. The complexity of EMS schedules coupled with unanticipated time-off and utilization of part-time employees made it difficult to engage the same crews on the same shift over the study period which led to less than 1/3 of the participants completing the entire curriculum. While we did not specifically look at team dynamics for this study, having changing crew members with different skill levels could have potentially changed the results compared to if we had been able to engage the same two-person crews throughout the curriculum. This likely highlights the real environment of pre-hospital providers and the changing crew dynamic depending on which crew members are paired together on a given shift. Additionally, the COVID-19 pandemic required an adjustment to the final training schedule. Only 1 of the 3 6-month trainings were held on time. The other two trainings were held 8 months from the initial training.
The local protocol change with regard to medication dosing led to some of the medication dosing errors, of which the majority resulted in underdosing.
A simulation-based curriculum on the management of paediatric seizure for EMS providers improved self-efficacy, knowledge, and performance of in various critical patient care actions in simulated settings.
1.
2.
3.
4.
5.
6.
7.
8.
9.
10.
11.
12.
13.
14.
15.
16.
17.
Thank you for agreeing to participate in this simulation study. We hope this will be a useful tool to help enhance paediatric resuscitation skills. Your participation in this study is completely voluntary. During the simulation portion of this study, you will be video recorded. These recordings will be used during the debriefing sessions and again for evaluation of the critical actions of each case. None of the data gathered here will have any impact on your current or future positions within Wayne Township and will not be utilized in any aspect of performance review. You are able to withdraw from the study at any point without any penalty or repercussions. These simulations will count towards 1 hour of paediatric continuing education. Completion of the survey will serve as your consent to participate in this research.
This initial survey will collect demographic information and questions regarding care for paediatric patients (age <16 years) based on your current protocols. There are no penalties for wrong answers so please complete them to the best of your ability.
Name:_____________________________________
1. What is your age?
2. What is your gender?
3. What level of training have you completed?
4. How many years have you practiced as an EMT-B/EMT-A/EMT-P?
5. Have you completed training in any of the following over the past 2 years?
6. How many paediatric patients do you care for per month?
Please circle a response for each of the following questions based on the 1–5 scale below
Survey scale: 1: very uncomfortable 2: uncomfortable
3: neutral 4: comfortable 5: very comfortable

| 7. | How would you describe your comfort level of your knowledge base when caring for paediatric patients? | 1 | 2 | 3 | 4 | 5 | |
| 8. | How would you describe your comfort level with caring for paediatric patients in general? | 1 | 2 | 3 | 4 | 5 | |
| 9. | How would you describe your comfort with caring for paediatric seizure? | 1 | 2 | 3 | 4 | 5 | |
| 10. | How would you describe your comfort with taking care a paediatric patient in respiratory distress? | 1 | 2 | 3 | 4 | 5 | |
| 11. | How would you describe your comfort level with technical skills when caring for paediatric patients? | 1 | 2 | 3 | 4 | 5 | |
| 12. | How would you describe your comfort with patient assessment skills in caring for paediatric patients? | 1 | 2 | 3 | 4 | 5 | |
| 13. | How would you describe your comfort with paediatric medication dosing? | 1 | 2 | 3 | 4 | 5 | |
| 14. | Describe your comfort level with providing bag mask ventilation to paediatric patients? | 1 | 2 | 3 | 4 | 5 | |
| 15. | How would you describe your comfort with caring for paediatric seizure? | 1 | 2 | 3 | 4 | 5 | |
| 16. | How would you describe your comfort with taking care a paediatric patient in respiratory distress? | 1 | 2 | 3 | 4 | 5 |
17. What tool do you use for calculating weight in paediatric patients?
18. Have you participated in simulation before?
19. If yes, please provide a short description of the scenario(s) you participated in
20. Would you be interested in having simulation integrated into your education curriculum?
21. I think simulation is a valuable tool in my training as an Emergency Medical Technician?
Please answer these questions to the best of your ability. There is no penalty for wrong answers.
1. When administering rescue breaths to an infant, the ventilation should be given over a period of:
2. Clinical signs of respiratory distress may include all of the following EXCEPT:
3. Late and ominous signs of respiratory failure include all of the following EXCEPT:
4. The initial impression consists of assessing all of the following EXCEPT:
5. Signs of increased respiratory effort include all of the following EXCEPT:
6. You arrive to find a patient actively seizing. What is your primary concern with this patient?
7. Your patient has a history of epilepsy. He has had a seizure and has not recovered the way he normally does, according to his family. While assessing this unresponsive patient, he suffers a second seizure. What is this called?
8. What defines status epilepticus?
9. You respond to a seizure. Your patient is a 3-year-old who is 15 kg. How much midazolam should you administer?
10. A 20 kg patient is experiencing an allergic reaction and you need to administer IM Epinephrine. You have 1 mg of epinephrine in 1 ml of solution (1:1,000). Your protocol calls for you to administer 0.01 mg/kg of 1:1,000 epinephrine IM. How many ml should you administer?

| # | Item | Yes | No | Time | Comments |
|---|---|---|---|---|---|
| 1 | Airway/breathing assessment (checks mouth, observes chest rise) | ||||
| 2 | Circulation assessment (Checks BOTH pulse and capillary refill) | HR BP Perfusion |
|||
| 3 | Neurological assessment (AVPU score) a. Assess pupil response b. Assess response to painful stimuli |
Credit for pupil response OR response to painful stimuli | |||
| 4 | Verbalize respiratory depression | ||||
| 5 | Apply supplemental oxygen appropriately (NC, NRB) | ||||
| 6 | Perform chin lift, jaw-thrust manoeuvre using appropriate technique (Airway manoeuvre) | NP/OP/Shoulder roll | |||
| 7 | Perform BVM ventilation using appropriate technique | ||||
| 8 | Perform BVM using appropriate rate (~20 per minute) | ||||
| 9 | Utilize ETCO2 during BVM ventilation | ETCO2 reading: Time placed: |
|||
| 10 | Verbalize seizure onset | Time: | |||
| 11 | Check bedside glucose | ||||
| 12 | Determine weight for weight-based dosing | Tool used: | |||
| 13 | Confirmation of appropriate dose based on weight using paediatric medication cards | ||||
| 14 | Two-person verification of medication used | ||||
| 15 | Administer first correct dose of midazolam per protocol *IV/IM/IN Midazolam/ (0.1 mg/kg) |
Time of 1st dose: | |||
| 16 | Administer 2nd dose of midazolam after 5 minutes Max 2 IV, Max 1 IN, IM |
Time of 2nd dose: | |||
| 17 | Verbalize diagnosis of status epilepticus | ||||
| 18 | Place IV/IO | Line placed: | |||
| 19 | Protocols Available and/or verbalizes use | ||||
| 20 | Reassessment of patient after medication administration | Time: |
Abbreviations: BVM – bag valve mask; ETCO2 – end-tidal carbon dioxide; IV – intravenous; IN – intranasal; IM – intramuscular; IO – intraosseous; NC – nasal cannula; NRB – non-rebreather.
(#) Critical actions out of 20 performed correctly.
Assessment completed by:
Signature______________________Date:___________