
Research shows inequity of access and provision of Simulation-Based Education (SBE) globally, perhaps especially for Simulation for Mental Health (S4MH). Integrated approaches to education improve outcomes, despite this, there is a lack of multi-agency education and service user/carer involvement. This innovative work involves service users and carers in the design, delivery and evaluation of an experiential, mental health, SBE programme for health and social care professionals, and multi-agencies. Highlighting important areas of inclusivity, equality and diversity provides valuable insight into the unique patient perspective and experience of their interactions with services and professionals, and knowledge, perspective, and role of the practitioner, considering the transition of the service user between services.
In a mixed approach, data was collected between November 2021 and March 2022 by pre- and post-participation survey of participants’ thoughts, beliefs, attitudes, behaviours and experiences of the programme. A thematic method was used for qualitative data analysis.
Completed survey response rate = 64%. Analyses constructed themes around safety, responsiveness, empathy, stigma and experience. Findings show increased confidence and understanding of roles following participation in the programme. Positive changes in empathy and respondents’ perspectives and behaviours were also reported.
Findings inform better integrated, co-ordinated systems and practices, demonstrating mutual benefits of service user and carer involvement, and value of multi-agency learning; increased knowledge, safety, empathy, mutual appreciation of roles and recognition in the value of lived experience integrated into learning. Implications for practice and mental health care are relevant to multi-agency professionals, service providers, service users, carers and families.
Simulation, Hybrid, Mental Health, Co-Production, Multi-Agency, Psychosis, Depression, Personality Disorder
Mental health (MH) problems are common, affecting one in four people each year [1,2]. Despite this, stigma and discrimination within MH and society are widespread, negatively impacting health and equality, and fuelling damaging misconceptions or stereotypes such as dangerousness [2,3]. Persons affected by MH are more likely to be a risk to themselves due to pain, distress or trauma [2,3], and are 10 times more likely to be victims of violent crime than perpetrators of it [4–6]. Stigma acts as a barrier to seeking support, receiving quality, safe, personalized care and thus affects experience and outcomes [7]. Education, engagement and integration are essential to overcome these challenges [7,8].
A huge disparity in resources, infrastructure, curriculum and technological support for Simulation-Based Education (SBE) is recognized across professions globally [9,10] with resultant inequity in provision and access, perhaps especially for Simulation for Mental Health (S4MH).
Technological inequality can be a major barrier to access and learning experience, unwittingly promoting social exclusion [11]. Weighted research suggests access to good technology and technological support combined with well-designed content and materials is all essential to afford engagement and stimulate curiosity. Simulation programme designs that address these themes reflect the needs of faculty and learners.
Integrated approaches to education and services recognize that persons experiencing MH problems come into contact with multiple agencies and professionals and reflect real-life situations and experiences of stakeholders, improve collaboration and provide opportunities for safe, purposeful learning. Despite this, there is a lack of multi-agency education. Integrated Care Systems [12,13], which draw upon a diversity of skills, knowledge and experience, provide opportunities for meaningful shared learning and growth. The intention is more efficient systems and improved outcomes essential in tackling inequalities and closing resource gaps. They support stakeholder engagement, inclusivity and a holistic approach whereby Service User(s) (SU) needs and experiences are central to safe, quality and preventative care [12,13]. Inclusivity supports collaboration and enhances satisfaction and achievement [13].
SU perspective has become an important global issue embedded within health and social care policy [8,14,15] and SBE standards [16]. Yet a study comparing SU and staff perspectives found only 7.5% of participating clinicians perceived SU as a valuable knowledge source, and SU referred to their involvement as tokenism that failed to create organizational change [9,17]. Recognizing the vital contribution of SU collaboration with practitioners will inform strategies to break down negative attitudes caused by lack of knowledge, education and organizational support [8,18].
Inclusive, holistic SBE design and delivery consider the diverse needs, abilities and experiences of both learner and facilitator to create more user-friendly programmes. Content must be authentic, relevant, useful and aligned with learning objectives, facilitating collaborative problem-solving and meaningful contextualized practice. Design quality alone will not guarantee learner experience, and unmotivated learners may struggle to engage [19]. Facilitation and briefing skills directly influence learner experience and achievement [20,21], emphasizing the importance of faculty training providing the capability to support learners’ meaningful reflection, critical thinking and transition learning to practice [22]. Effective debriefing is highly prized by learners, providing opportunities to voice ideas and perspectives, support discussion, reflection and self-assessment of learning to cement knowledge acquisition [22]. Facilitation and debriefing are considered critical components of SBE, requiring skill and an informed approach to elicit active participation and achievement of objectives [22–24].
Learners are motivated and empowered by facilitators participating as co-learners in the learning process, increasing engagement and performance [25,26]. Observational roles provide meaningful and engaging opportunities for learning that lead to positive educational outcomes [27,28]. Observers in non-directed roles have been found to experience significantly less satisfaction compared to learners using directive tools such as checklists. Therefore, roles need to transform from passive to active participators, capitalizing upon learner experience and engagement to achieve better learning outcomes [27]. Observers highly value learning from peers’ experiences and errors [28], through modelling and imitation of positive behaviour [29]. However, increased anxiety has been found in participants being observed [30], highlighting the importance of creating a psychologically safe SBE environment.
Simulation best practice considers risk management within design and delivery to establish a safe physical and psychological environment for all SBE activities [16] including adherence to health and safety protocols of the controlled environment within which simulation is intended. The process of positive risk taking encompasses a personalized approach, focusing on preserving choice and control to accomplish change and personal growth [31]. Psychological safety [32] refers to feeling safe without fear of repercussion to share thoughts, make mistakes, take risks and request support [33]. Learner perceptions of safety affect willingness for active participation and engagement, directly impacting learning outcomes [34]. Technological barriers, as described here, present new challenges to faculty, whereby familiar strategies to engage and support learners may not be adequate. For example, in virtual simulation, a lack of physical presence means cues such as body language, eye contact and opportunity to ‘sense’ how a learner may be feeling are much harder to ascertain [34]. Pre-course material including information packs and video have been shown to boost learning, motivation and enhance psychological preparedness [27]. Notably, adequate human resources and experience ensure a responsive approach that observes learner verbal and non-verbal cues to trigger planned actions to prevent harm [35].
The objective of the S4MH project was to design, deliver in three locations across the southeast and evaluate an innovative regional 1-day S4MH programme. Exceeding this, three distinct hybrid 1-day programmes (psychotic, depressive and personality disorders) were delivered with combined in-person and online participation, as part of the Health Education England for Kent, Surrey and Sussex regional simulation and human factors project. Each programme addressed a separate theme, and three sites across Kent were selected to host the programmes:
The programmes were targeted towards multi-agency professionals working in acute and community services. Participants included front-line Police Officers and registered healthcare professionals: Paramedics, Occupational Therapists, Nurses, Social Workers, Pharmacists, Doctors, and Speech and Language Therapists. Each programme was designed to accommodate a minimum of 10 and a maximum number of 20 participants.
Design and delivery involved working in co-production with service users and carers, referred to here as Expert(s) By Experience (EBE). EBE recruitment entailed close collaboration with existing partnerships and advertisement through national organizations and social media. Within the design phase, initial engagement encompassed semi-structured interviews with designated clinical faculty (Table 1, Figure 1) to explore the EBE’s unique lived experience and their interactions with front-line services, and health and social care professionals. This process required an appreciation of where they were in their journey, their perceived ability to be involved, what involvement would look like, support and management of mutual expectations. Learning from this process informed design and delivery and helped to define the targeted audience. Programme themes were identified through the authors’ clinical expertise in combination with EBE’s unique insights: effective communication, involving service users and carers in treatment planning, use of language, conveying empathy towards service user and carer, and working to reduce mental health stigma. EBE participated as co-faculty to support effective delivery and achievement of the learning objectives, and as co-learners, to help contextualize the learning experience.

| ‘I don’t expect everyone to love me, but at least respect me.’ |
| ‘One doctor just kept throwing anti-depressants at me – he was after the cure, not the management’. |
| ‘Our GP was brilliant because they spoke to us and not at us … they really listened and demonstrated understanding’. |
| ‘The first visit to the psychiatrist was devastating; we never expected the response we experienced … they said to her ‘If you are going to cry you are wasting my time’. I felt angry and let down.’ |
| ‘I was discharged with no information about what would happen next. No-one explained what support was available, no-one thought to ask how I would manage, I was going home to an empty house … this just reinforced the feelings of abandonment.’ |

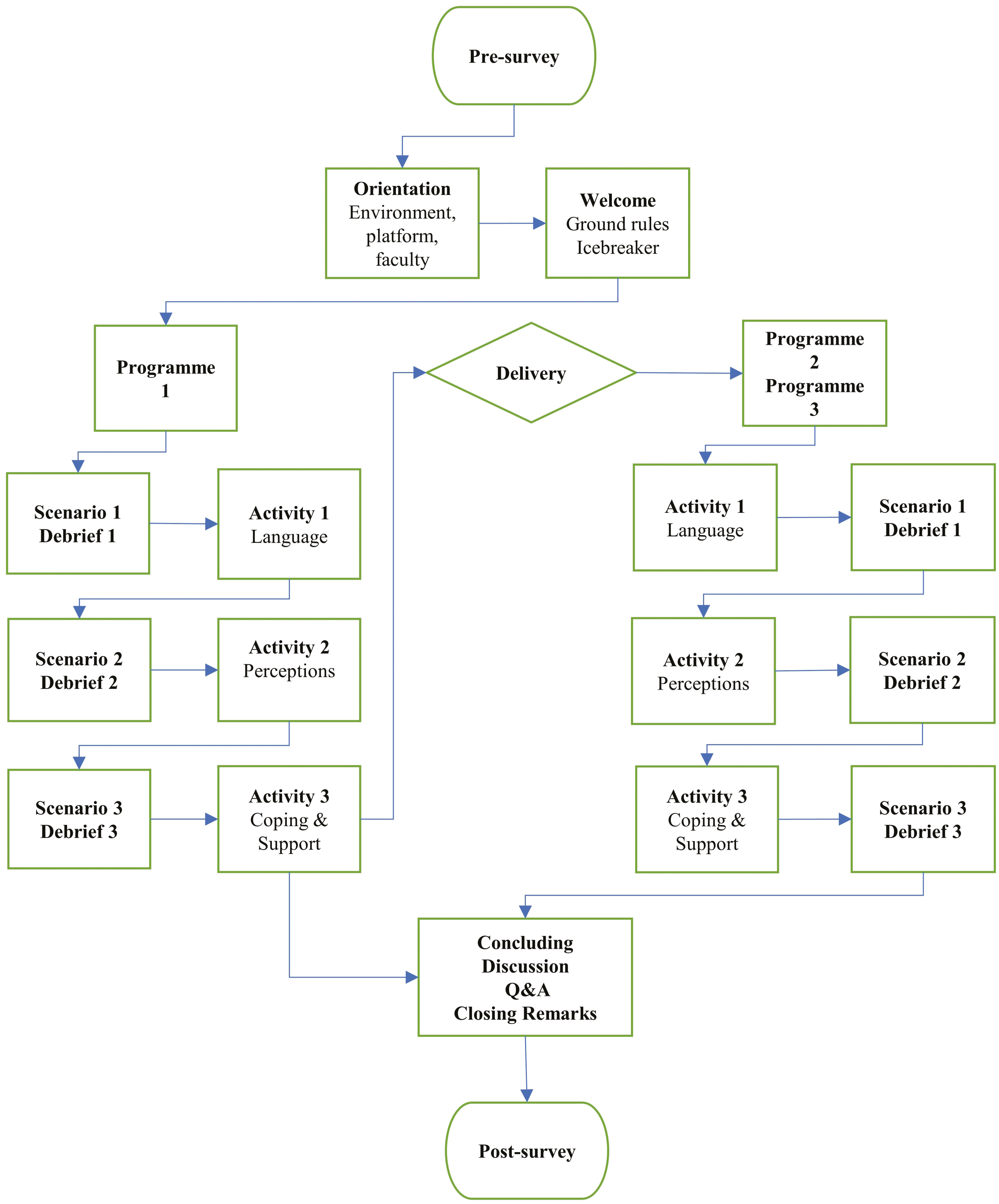
Overview of the three 1-day programmes
Many aspects of the EBE experiences stayed with them, and significantly, preparation supported the development of psychological safety by means of pre-event focus groups facilitated by the same designated faculty.
The three programmes were piloted in November 2021. Each programme combined experiential activities and clinical simulated scenarios, followed by a debrief. Activities and simulated scenarios were designed in alignment with the learning objectives (Table 2), and explored communication, beliefs, attitudes, behaviours, roles, practices and lived experience in relation to the programme theme. Content supported diversity and provided narratives to instil curiosity, discussion, problem solving, reflection and learning. Quality assurance of activities and scenarios encompassed peer review by experienced simulation faculty, subject matter experts and EBE.

| To develop: |
|---|
| Recognition of mental health stigma, associated behaviours, attitudes and their impact on outcomes |
| Knowledge and confidence in the appropriate management of persons affected by psychotic, depressive and personality disorders |
| Empathy for persons affected by mental health disorders |
| Situational awareness in risk management and assessment when working with persons experiencing mental health challenges |
| Appreciation of interdisciplinary and multi-agency roles and practices |
| Interdisciplinary and multi-agency integrated collaborative learning |
| Identification of the value of lived experience integrated into learning |
All participants participated in the experiential activities and briefings. Activity breakout groups were optimally balanced to reflect the diversity of participants.
Experiential activities were designed to develop cohesion, psychological safety and preparedness for the simulated scenarios and debriefs (Figure 2).

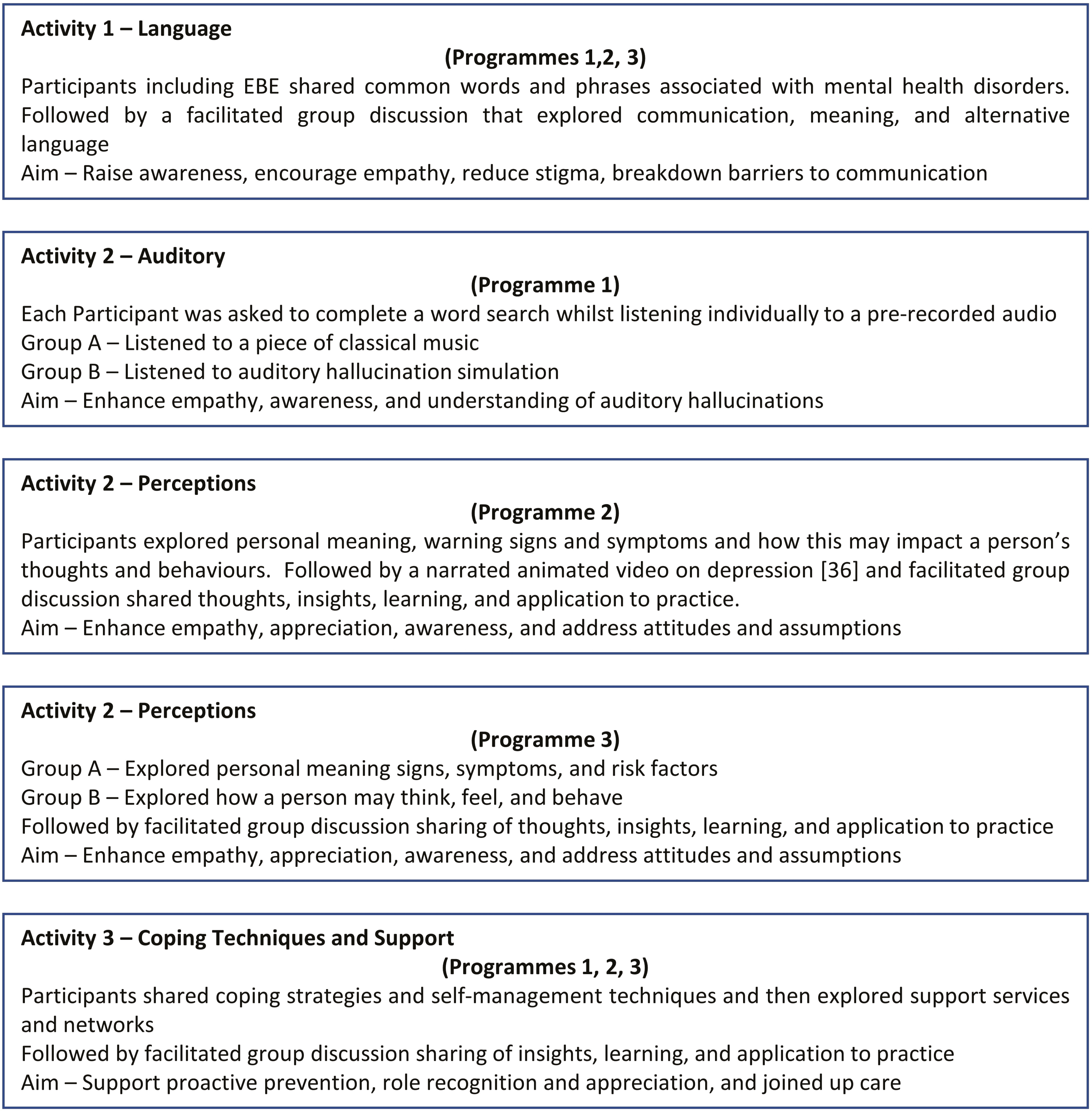
Project experiential event map
They addressed community and acute cases, appropriate to participants who had been carefully recruited so that a bespoke event was tailored to their needs, experiences and abilities. This was all designed to capture an SU/carer journey, the transition between community and acute care, and to examine the roles and practices of participating professionals.

| Scenario 1 | Scenario 2 | Scenario 3 | |
|---|---|---|---|
| P1 and P2 – Sequential Simulation [37] | |||
| P1 | Community setting: At home Helen has experienced a deterioration of mental health, withdrawing from social contact, acting out of character, and has become increasingly isolative. Carer is concerned and has accessed the property. Helen appears distressed, and reports people are trying to get into the property. Carer calls 999 to summon emergency responses. |
Psychiatric in-patient setting: Carer attends ward review with Helen Helen has been receiving treatment for the past 6 weeks. Ward staff have noticed a slight improvement in her mental health. Helen requires encouragement and verbal prompts to take medication. At times, Helen still appears distressed, responding to visual/auditory hallucinations. Helen spends a lot of time isolating in her room, she does not initiate engagement with other service users or staff. Helen currently requires support to manage her activities of daily living. |
Community setting: GP Practice Helen has been discharged from hospital and is attending a GP appointment with her carer for review. |
| P2 | Community setting: Paul’s home Paul has called a support charity phone line. He has told them he plans to end his life. After speaking with them for a while, he has agreed not to act on his plan. The charity summons the support of the emergency services who attend Paul’s home. |
In-patient Acute Physical Health Hospital Ward Paul is an inpatient on a physical health ward. He was admitted following a period of high blood sugars and borderline diabetic ketoacidosis. Leading up to admission he was in crisis and had planned to end his life. Paul remains low in mood. He has received treatment and is medically fit for discharge. Paul is awaiting Mental Health review. |
Community setting: GP Practice Paul presents to the GP with low mood, lack of motivation, and anxiety |
| P3 Individual Simulated Cases | |||
| P3 | Community setting: Alex’s home Alex was due to see a mental health practitioner at home today. The practitioner called in sick and therefore is unable to attend the schedule appointment. Alex has sent a text to the practitioner stating they intend to end their life. Responders attend their address. |
Community setting Jamie has been experiencing extreme anxiety. Today, they are attending an initial assessment appointment with the community mental health team. |
Community Setting: GP Practice Morgan has a diagnosis of emotionally unstable personality disorder. Recently, they have been discharged from the community mental health team, following therapeutic input, which Morgan said they have found helpful. Morgan has presented to the GP with their discharge letter, seeking support from the GP. |
Note: Simulated scenarios were fictional creations based on a generic combination of multiple cases and lived experience
Trained simulated patient(s) (SP) recruited through an active SP programme portrayed SU and carer roles as part of an authentic learning experience. SP participated in debriefings providing feedback to learners. A combination of online and in-person participants engaged in the simulated scenarios. Participants were required to actively engage with SP as they would in their professional role in the assessment and management of persons affected by MH. All other participants were observed via video stream. Online and in-person participants then regrouped together for a debrief led by faculty skilled in the process of debriefing.
On the first engagement, semi-structured interviews with EBE involved information provision regarding the nature and background of the project, potential risks and benefits, and suitability for participation. This process helped build mutual rapport and trust that contributed to psychological safety and was, and continues to be, sustained throughout the project. EBEs were free to withdraw and opt out of the project at any time without precondition or explanation. Informed consent was sought and provided on EBE engagement, at different stages throughout the project, and prior to the use of related information. Following the pilot of programme three, 1:1 meetings were organized directly between EBE and a clinical psychologist. This provided a supportive space, independent of faculty, where EBEs could reflect on their experience and provide additional feedback. EBE informed consent was obtained for learning to be anonymized and shared with faculty to inform future work.

| Hazard | Persons at risk | Current control measures | Risk rating | Additional control measures required |
|---|---|---|---|---|
| Tech equipment available/not working | Participants Faculty |
1. Participants notified of required equipment 2. Faculty and venue – pre-checks including A/V |
High | 1. Admin check on registration Orientation to the platform, tools and hybrid environment |
| Connectivity | Online Participants Faculty |
1. Meeting platform MS teams agreed and participants pre-notified | High | 1. Allow pauses/time for clarity to mediate internet drop-out 2. Participants to keep mics off unless talking |
| Camera presence or not | Online Participants | 1. Protocol re camera presence agreed and participants informed | Medium | 1. Revisit protocol in housekeeping/boundaries |
| Confidentiality/ Recording of the event | Online/ Face-to-Face Participants | 1. Protocol re-confidentiality agreed | Low | 1. Revisit protocol in housekeeping/boundaries |
| Online Communication – No Physical Prescence (Lone Working) |
Online Participants Faculty | 1. Participants encouraged to take care of their well-being during the meeting 2. Psychological safety teams room/support accessible 3. Confidentiality protocol agreed 4. Protocol re camera presence agreed 5. Use of teams background to provision privacy |
Medium | 1. Designated faculty follow-up with experts with lived experience after the event |
| Risk of Fatigue (MSK/ eye strain) | Online Participants Faculty |
1. Scheduled breaks and rest periods | Medium | 1. Designated faculty encourage participants to stretch and look away from the screen at regular intervals |
| Issues with Covid 19 | Face-to-Face Participants Faculty | 1. COVID protocol agreed (face-to-face participants, faculty, venue) | Medium | |
| Risk to Psychological Wellbeing | All Participants Faculty | 1. Psychological safety protocol agreed | Medium | 1. Virtual private space – support accessible to all participants 2. Post event check in with EBE by designated faculty 3. Post event – 1–1 meeting planned between experts by lived experience/psychologist 4. Designated faculty provided support to SP pre/post and during the programme(s) |
| Data Protection GDPR |
All | Protocol agreed on the following 1. Anonymization of data sets 2. Controlled storage access of data 3. Permission to use/store data 4. Retention 5. Housekeeping |
Low | Faculty mandatory DPA/GDPR training |
Data security/GDPR was carefully managed and related to process and control, confidentiality, and anonymity. Data dissemination of findings directed towards SBE audiences via workshops, oral presentations, regional groups, newsletters and publications were discussed, agreed and revisited with EBE as appropriate. Pre-programme information covered confidentiality, right to withdraw, expectations of participation and informed consent to the use of audio/video and anonymized data for publication. Each programme delivery incorporated participant access to a private online space with supporting faculty, if required. Risk management planning and ownership were shared across the S4MH faculty team.
A convenience sample was selected from the targeted areas of Kent, Surrey and Sussex, and baseline data were gathered regarding demographics and professional background which assisted recruitment. Inclusion criteria included multi-agency and post-registered professionals (Table 5), working with adults affected by one of three MH disorders within the targeted geographical area. The sample was accessed through multimedia marketing via social media, networking and direct contact with stakeholders.

| P 1 Psychotic disorders, N = 19 | P2 Depressive disorders, N = 10 | P3 Personality disorders N = 16 | Total number of individual participating | ||||
|---|---|---|---|---|---|---|---|
| Online | In-person | Online | In-person | Online | In-person | ||
| Experts by lived experience | 2 | 2 | 2 | 3 | |||
| Police Officer (Front line) | 6 | 1 | 1 | 2 | 9 | ||
| Paramedic | 3 | 1 | 1 | 1 | 1 | 6 | |
| General Practitioner | 0 | 1 | 3 | 4 | |||
| Psychiatrist | 0 | 0 | 1 | 1 | |||
| Nurse | 1 | 2 | 1 | 3 | 7 | ||
| Occupational Therapist | 4 | 2 | 0 | 1 | 7 | ||
| Speech and Language Therapist | 1 | 0 | 0 | 1 | |||
| Mental Health Practitioner | 0 | 0 | 1 | 1 | |||
| Suicide Prevention Officer | 0 | 0 | 1 | 0 | 1 |
In-person numbers may have been affected by the COVID pandemic; however, the success of the events led to the planning of a further 100% online course.
Data were collected between November 2021 and March 2022 by means of survey pre- and post-participation. To ensure survey anonymity, respondents were required to generate a unique code that could be cross-referenced for pre–post analysis. Survey items included Likert 5-point scale and open questions to evaluate the impact of the S4MH programme upon knowledge, confidence, understanding of roles, empathy and experience of participation.
Manual analysis involved familiarization through reading and re-reading to search for understanding. Through the process of coding, ideas and insights were reflected on, and data were systematically categorized by the author (IC). The next stage highlighted patterns, relationships and explored meaning. Some codes were merged, and themes were generated by (IC) to capture meaning. Data and themes were revisited, amended, and then defined and named. The final step involved a write-up that provided Illustrations by verbatim quotes [38,39]. Data analysis validation included peer review.
All participants were asked to complete surveys. Twenty-nine of the 45 participants completed both pre- and post-surveys giving a completed survey response rate of 64% (Table 6).

| Programme 1 | Programme 2 | Programme 3 | ||||
|---|---|---|---|---|---|---|
| Pre | Post | Pre | Post | Pre | Post | |
| Total questionnaire responses received | 18 | 14 | 8 | 12 | 17 | 11 |
| Excluded: duplicate entry for same participant | 2 | 5 | ||||
| Completed only pre- or post-assessment | 3 | 1 | 3 | 2 | 6 | |
| Analysed paired responses | 13 | 5 | 11 |
Participants were asked to provide feedback on their experience of faculty and the programme:
Analysis of data suggests respondents did not perceive technical challenges to be a barrier to experience, learning or engagement. Participant responses revealed a statistically significant change in confidence and understanding of roles.
Analysis of survey-free text concerned thoughts, beliefs and attitudes. Respondents across all events shared thoughts when being called to attend an acutely unwell person. Most respondents identified the safety of the SU, carer and attending professional as a key consideration. Pre-surveys reflected views of potential risk:
How acute is acute? How will it present itself? Are they a danger to themselves or others? (P1R3)
Risks? Where is the person? Is anybody else with the person? (P1R7)
And Are they physically safe? Are they a risk to me or my colleagues? (P3R3)
Post-survey responses highlighted actions around support and prevention:
Being present, active listening, and understanding protective factors. (P2R8)
Listen, ask questions, be aware of physical triggers as well as mental ones. (P3R3)
Is there a care plan? Is this a new episode or are they known to MH Services? Who will be the key responders? Do we need emergency services? The need to get background information to aid formulation. (P1R2)
Relatives and carer need to be involved where possible. (P1R11)
The second theme related to participants’ ability to help the SU in crisis. Many respondents reflected on their perceived level of confidence and ability to react appropriately and positively. A presence of apprehension was noted in several pre-survey responses:
Will I say the wrong thing? Will I help or hinder? (P1R3)
Will I make matters worse? Panic, fear. (P3R4)
Am I capable of helping them? How quickly will the services I refer them to respond? (P3R8)
In contrast, post-simulation responses focused on supportive actions and behaviours:
Listen, stay calm, patience, safety, and listen again. (P1R3)
I must listen to what they have to say, I must stay calm, I need to sit and talk with them not stand over them. (P3R4)
Build trust, keep patient safe, keep patient informed. (P3R8)
Respondents shared their beliefs about persons affected by psychotic, depressive or personality disorder(s). Pre-responses:
I don’t think I believe anything – I just feel very compassionate towards them and patient because of the distress they could be experiencing, and how out of their control the psychosis must feel. (P1R4)
It’s a waste, it hurts others, it sometimes feels like the only choice for people, I am not judgmental about it. (P2R11)
These patients have a mental health condition which can be challenging for both
them and the professionals trying to help. (P3R22)
Increased empathy was reported by several participants following participation:
This session made me more empathic towards someone sectioned with a mental health condition.
‘I feel I understand things from the patient’s point of view better after this course.’ (P3R22)
Analysis provided some insight into existing beliefs and attitudes around existing mental health stigma and stereotypes:
We need to work towards eradicating the stigma around depression and suicide. (P2R4)
They are highly stigmatised against, and they are considered to be bad people who are impulsive and manipulative. (P3R13)
In contrast, stigma was regarded in several pre-responses involving negative attitudes and beliefs around personality disorders:
Oh no, this is going to be time consuming, they are going to be draining, I think they are going to find my Achilles heel to get back at me. I’m not looking forward to this. (P3R6)
How draining will this be? (P3R13)
In some responses, psychotic disorder was associated with dangerousness or substance misuse:
They need help to manage themselves and others safely. (P1R8)
What has caused this? Social drugs or alcohol? (P2R7)
Are they violent? have weapons? drugs, or alcohol? (P1R9)
Post-survey responses highlighted changes of perspective:
They are unwell, they need to be listened to and heard, their needs need validation, understanding their preferences, what is triggering/calming? And, to not jump to conclusions. (P1R2)
I have seen personality disorders with a different view, I found the workshop has changed my way of thinking with personality disorders. (P3R2)
In their accounts, nearly all respondents enjoyed the multi-agency learning experience:
The multi-agency approach, this set the event apart from any training that is already
running in house. (P1R3)
I enjoyed the number of agencies involved and the amount of interaction. (P3R14)
Really helpful and enjoyable to be working with other professions and hear their side of things. (PR18)
Many respondents emphasized the authenticity of simulated scenarios involving SP, highlighting their enjoyment and usefulness of the simulated learning experience:
Overall, I thought it was very informative, the scenarios were excellent! (P2R9)
The realism of simulation and authenticity of actors. (P1R22)
I really enjoyed the immersive ‘real life’ simulated scenarios. (P2R8)
I found the event very informative and illuminating … there was so much I didn’t know about the acute response to a psychotic incident. (P3R13)
I learnt more about personality disorder and the effects, and how to respond better.
I think its brilliant, it allows people to be put in situations without actually involving a patient, so they get to learn how to respond without it being detrimental to a service user. (PEB1)
One respondent concluded:
The activity gave good insight to what it is like for someone who is hearing voices, I noticed I became very competitive short-term but realize long-term the stressful impact it has on a person’s wellbeing and health. (P1R18).
Respondents valued the simulation debriefs that elicited purposeful discussion and reflective practice:
The experience itself was fantastic, meeting people from different working backgrounds and being able to talk openly had a great impact. (P3R13)
The case studies and simulation scenarios acted for us to provoke discussions which has impacted the way I work.
Observation and participation in the simulated scenarios triggered a deeper appreciation of perspectives, roles and practices:
My practice has definitely changed I have a better understanding of other roles and beliefs of their approaches in other disciplines. (P1R4)
Finding out different people’s roles was a real eye opener. (P3R15)
It has given real insight into what each responder/ service provider can and can’t do and has given us all an insight as to how that can impact other providers and the service user. (PEB2)
Several respondents reflected on the value and enjoyment of EBE involvement:
Very interesting learning more about what patients may be experiencing, gaining insight into disorders and the lived experience. (P1R20)
Another enjoyed the interactive nature, and involvement of individuals lived experience. (P3R19)
EBE described their experiences of involvement:
Not only was I listened to, but my answers were reflected at me to check that what I was saying was what they thought I was saying. It was a project that felt very worthwhile, and I just wanted to be involved in it. (PEB2)
My personal experience as an expert patient was very much listened to and taken on board throughout the project. It’s a worthwhile and brilliant experience, I felt supported, I felt really cared about, I felt listened to. Nothing was a surprise which helped … I felt very safe. (PEB3)
This pilot is, to the authors’ knowledge, the first of its kind in its interdisciplinary, multi-agency and multi-faceted approach to MH SBE, making this a unique and original piece of work, reliant on the diverse perspectives, expertise and shared knowledge that informed participants’ understanding. The work also places simulation scenarios as a component of experiential learning activities in a multi-faceted event design.
Participants reflected on their experiences of the S4MH programme, and analysis revealed that 100% of respondents felt supported by faculty throughout, and faculty to participant ratio was satisfactory, allowing for supervised practice within a safe, supportive, simulation environment [16]. Faculty participating as co-learners assisted engagement and performance [25,26], and clearly defined roles, responsibilities and expectations contributed to the efficiency of delivery and overall experience of participants [35].
Pre-testing of technology, equipment, and use of online platform helped minimize technological challenges, enhance user experience, and prevent the risk of drop-out [40]. Disparity in platform user tool functions existed between some users, which may have been due to freeware access or user privilege. Responsive faculty effectively supported participants in overcoming any residual minor disparity in platform functionality issues during the programme.
The multi-faceted design was an important feature that allowed learners opportunities for both active observation and participation. For example, tasks given to observers of simulated scenarios via video link encouraged active meaningful engagement and experience, as evidenced in previous studies [26,27,29]. Hybrid delivery supported accessibility to MH SBE through combined online and in-person participation, affording flexibility, choice and control to participants, which improved inclusivity and equity [11]. Participant preference resulted in a majority of 82% attending online and 18% in-person, possibly influenced by experiences and prevailing attitudes of the pandemic in 2021.
Data show improved responsiveness and increased ability in safety planning and management of persons experiencing acute MH difficulties. We are reassured that respondent increased knowledge corresponds with their perceived increased confidence, avoiding a confidence/competence mismatch, and furthermore, this may support the application of knowledge into practice.
Effective risk management incorporated risk assessment and identified potential hazards addressed through the formulation of risk controls, and systematic review ensured a safe learning environment for collaborative learning [16]. Moreover, risk management considered diversity among participants through thoughtfully designed activities that elicited communication of ideas, perspectives and language associated with MH, which established common ground between participants. Pre-programme information assisted psychological preparedness [27] and possibly influenced self-selection and initial engagement [19]. The registration process and ice breaker facilitated user efficiency and experience through orientation to the hybrid simulation environment.
Following participation in the S4MH programme participants had an increased appreciation of roles and practices, triggered by observation and participation in the simulated scenarios where participants practiced communication and actions in supporting persons affected by MH. Experienced faculty participating as co-learners within the learning process assisted engagement and performance [25,26], while debriefing empowered and supported participant voice and active engagement [22–24]. Debriefing was highly valued by participants and elicited self-reflection on performance and actions, feedback and meaningful learning. Furthermore, reflection on roles, responsibilities and challenges achieved greater appreciation of the SU, carer, and professional perspective and experience.
This outcome considers how the simulations created and sustained these interactions within a psychologically safe environment. Notably, the private online space with 1:1 faculty support was not utilized during the programme(s), further suggesting participants felt safe throughout. These findings demonstrate the mutual benefits of cohesive, multi-agency MH SBE programmes that drive inclusivity and the delivery of safer, integrated, preventative care [12,13].
The design strategy provided an inclusive and transparent approach, embracing EBE involvement central to the process of design, delivery and evaluation, enhancing satisfaction and achievement [13]. Engagement encompassed equal partnerships with EBE participating as co-faculty and co-learners. EBE conveyed their participation and involvement as extremely worthwhile, they felt supported, empowered to have their voices heard and that participation had led to positive outcomes. These results contradict previous published studies where complex relationships between service user involvement and tokenism were established [17]. Findings from this study signify positive outcomes for both service user/carer and professional participant, necessary to break down barriers to involvement [8,18].
The present study contributes to the vast body of evidence that stigma is active and present across healthcare disciplines and agencies [2,3]. This work demonstrates how a holistic and inclusive approach to learning that embraces diversity can positively change attitudes and behaviours towards persons affected by MH, highlighting the value of MH SBE in tackling stigma and driving cultural change to improve outcomes.
Positive change was found in respondents’ increased ability to empathize with persons affected by MH following participation in the programme. An explanation of these findings considers the impact of real-life stories providing meaningful contextualization of what it might be like to walk in another person’s shoes. This idea is further supported by the finding that respondents perceived EBE involvement as being one of the most useful and enjoyable aspects of the learning experience. This study demonstrates the importance of inclusion and contributes to existing evidence relating to the involvement of EBE in design, delivery and evaluation of MH SBE in healthcare [8,14–16]. These results provide new insight into the mutual learning benefits of EBE and multi-agency professional involvement in MH SBE. This is significant and could be a driver to viewing EBE involvement in a new light, for it has the potential to benefit not only the multi-agency professional but also the person with lived experience and faculty. In turn, this may lead to improved collaboration, satisfaction and enhanced relationships between professionals, SU and carer(s), and furthermore improve the use of services and their efficiency.
Limitations of this study concern data collection that returned duplication of a small number of responses. In retrospect, the authors regret not disabling multi-responses that would have prevented this. Steps taken to ensure anonymity produced cross-referencing challenges in data collection. The issue of self-selection could be addressed through future research, which should consider the same study on a larger sample to achieve generalizability.
Further studies are indicated to extend current findings of EBE perspectives and experiences of MH SBE. Future research is needed to explore the impact of MH SBE involving multi-agencies and EBE upon service provision and use. Finally, engaging the perspectives and attitudes of SU/carers and multi-agency professionals is crucial to help overcome barriers to inclusivity, equity and diversity in MH SBE.
None declared.
With special thanks to Sarah Keeling-Smith Regional Simulation Project Administrator, Kelly Marie Lee, Susan Sargent Hughes, and Mark Hughes, EBE, Dr Ruth Charig, Clinical Psychologist, The Digital Innovation Centre team, Folkstone, Verena Holmes Building team, and Rowan Williams Court team, Canterbury Christ Church University.
HEE KSS.
None declared.
None declared.
None declared.
1.
2.
3.
4.
5.
6.
7.
8.
9.
10.
11.
12.
13.
14.
15.
16.
17.
18.
19.
20.
21.
22.
23.
24.
25.
26.
27.
28.
29.
30.
31.
32.
33.
34.
35.
36.
37.
38.
39.
40.