
The use of mixed reality in simulation-based education (SBE) has been on the rise in the healthcare field; however, elements of human interaction, such as communication, may be missing. The implementation of hologram technology, a type of mixed reality, allows learners to apply their nursing skills in a safe environment while practising communication skills.
Embedded participants (EPs) are role players (actors) in a simulation [1]. A tele-EP is not in the same physical location as the learners during a simulation and can be present in the form of a telehealth robot, tablet, hologram or live stream. When substituting for a simulated caregiver, tele-EPs have been referred to as ‘pop-up parents’ [2]. A hologram, conversely, is a projected three-dimensional image that can beam into a scenario or be pre-recorded and interact within the environment [3] (see Figure 1). The recorded video-like image has realistic pauses, based on natural conversation, allowing time for participant interaction. While the hologram technology currently does not include artificial intelligence (AI), the natural pauses and life-like projections mimic a live person. These images, in the form of a hologram, allow for simulation consistency without relying on actor availability (see Figure 2). With high-fidelity simulation and the use of a tele-EP, learners can demonstrate communication skills, behaviours and attitudes while conducting interviews and developing a plan of care [1].

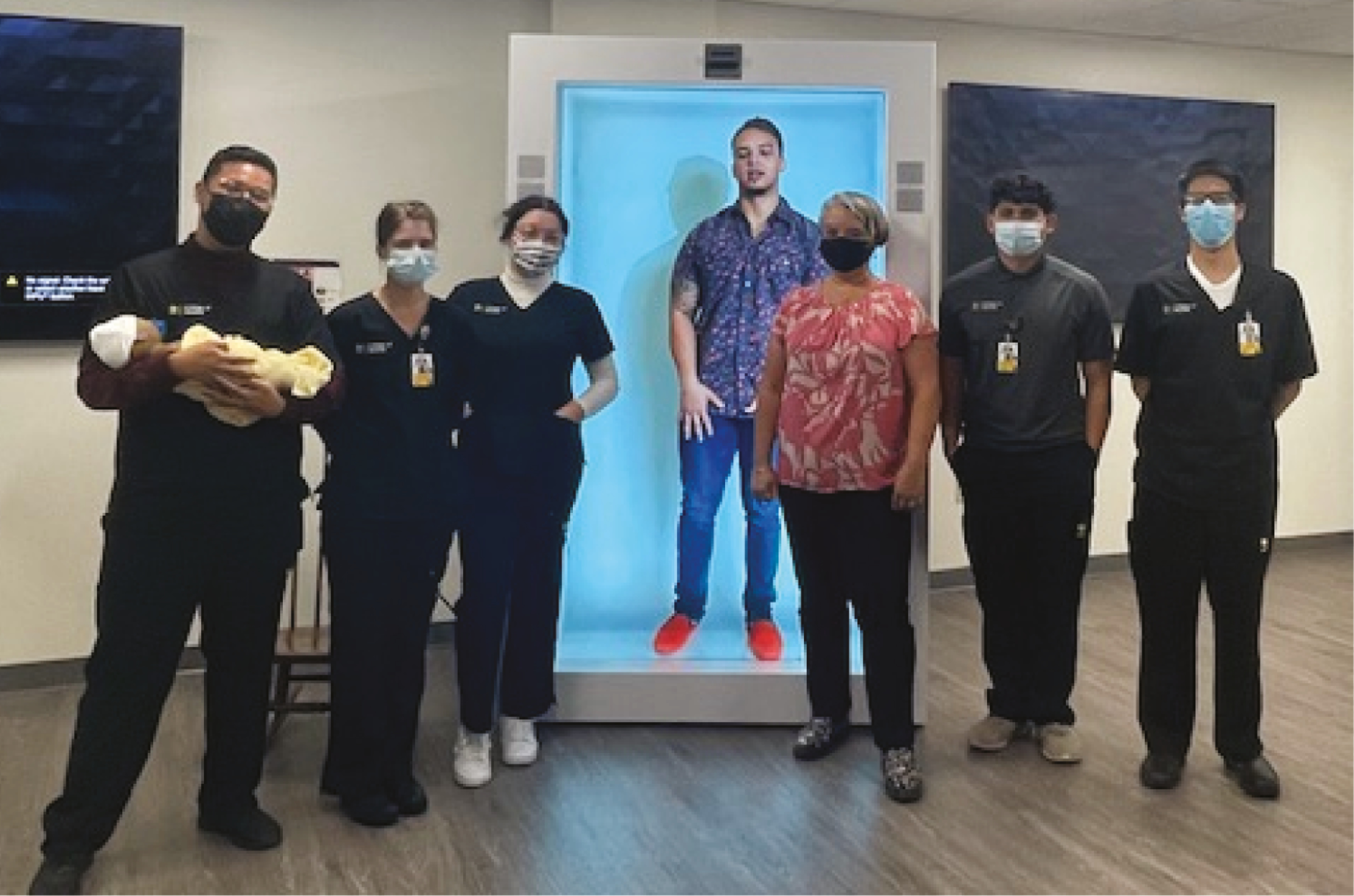
‘Pop-up parent’ virtual tele-EP as a hologram


Participants interacting with the hologram.
The purpose of this study was to explore the feasibility of a tele-EP as portrayed via a hologram.
A small convenience sample of prelicensure student nurses at a university of substantial size in the United States was invited to participate. SBE was a course requirement; however, participation in the completion of research surveys was optional. Inclusion criteria included active enrolment in a clinical practicum course.
Following Institutional Review Board approval, students were recruited. Participants consented to the study during the pre-brief which included a report, information regarding the potential use of tele-EP and that the father in the scenario may be present. Participants were assigned to a tele-EP via a hologram. The Principal Investigator was not the faculty of record for the didactic course.
A published and validated healthcare disparity-infused infant scenario [2] served as the simulation. An EP was added to augment the interaction with the parent. A structured debrief followed.
Demographics. Information collected includes gender identity, race, ethnicity, age, marital and parental status.
The Simulation Effectiveness Tool-Modified [4] (SET-M ). This tool explored learners’ perceptions of simulation effectiveness. The 19-item instrument evaluated students’ learning and confidence throughout the SBE. Participants scored the responses using a Likert scale ranging from 1 (do not agree) to 3 (strongly agree) [4].
Actions, Communication, Teaching in Simulation (ACTS). The ACTS Tool [5] is an objective way to evaluate EP contributions to the SBE. Actions were evaluated on a scale from 0 (inadequate) to 6 (outstanding). The instrument is valid and reliable with Cronbach’s alpha of .93 and Pearson’s R of .91 [5].
The feasibility pilot subset included five students, who were blind to the type of tele-EP. Participants were 22 years of age (n = 4, 80%), mostly males (n = 3, 60%), Asian (n = 2, 40%), White (n = 2, 40 %) and Black/Afro-Caribbean (n = 1, 20%). The majority identified as Hispanic (n = 3, 60%). None were married or parents.
The overall SET-M total mean was 49, and the individual subscales mean ranged from 2.6 to 3.
ACTS Tool’s mean score was 26 for the tele-EP hologram. The lowest subscale mean score for interacting with participants was 4 (adequate).
The results indicate that the tele-EP via a hologram was overall effective, and the initial evaluation resembles the evidence in the larger sample [2]; however, a small sample size affects the identification of significant relationships. Further research is needed to establish the practicality of using holograms as EPs in SBE.
Educators may be able to enhance simulation scenarios by incorporating tele-EPs. Tele-EPs have the potential to enhance community engagement, providing opportunities for volunteers to interact with learners while being remote. A notable pro of the holographic tele-EP parent was the possible increase in the fidelity of the simulation scenario and the similarity of communication to that with patients in the clinical setting. However, there was a lack of ability of the tele-EP to be able to respond to learners due to being a recorded hologram without AI. Communication and interaction with the participant are important elements to maintain as they can potentially impact learning. Cons included the fiscal implication of technology-dependent scenarios and resources to sustain consistent elements in every SBE.
Further research is needed to see how holograms can affect learning. Interactions between participants and the tele-EP parent were adequate, but limitations occurred. However, future improvements with AI in such technology are promising. Future iterations may also improve the size of the technology.
The study team wishes to acknowledge the College of Health Professions for the use of its holoportation technology (https://healthprofessions.ucf.edu/rehabilitation-innovation-center/).
DAD consented participants, collected data, analyzed data and wrote submission, MA edited and wrote submission, BH hologram preparation, edited and wrote submission, Student Research Team all contributed to the background and writing of the brief: JVA edited and wrote submission, EGS edited and wrote submission, AWG edited and wrote submission, AV edited and wrote submission, AW edited and wrote submission.
None.
None.
IRB was obtained and all learners consented verbally prior to the SBE.
None declared.
1.
2.
3.
4.
5.