
The critical care environment is stressful with complex clinical cases and high levels of workload [1]. Adequate exposure to various clinical experiences is essential to develop effective clinical reasoning skills [2]. Taking into consideration the risk of clinical practice mistakes and the importance of patient safety, simulation is an effective method to immerse learners in scenarios that mimic clinical situations with focused learning opportunities. Guided reflection through reflective learning conversations following simulation activities is recognized as an effective method to develop clinical reasoning skills [3]. We describe a co-design process to develop a simulation guided reflective learning conversation model to optimize the clinical reasoning skills for critical care nurses attending simulation-based activities.
A co-design working group of 10 critical care nurses of varying levels of seniority, experience, nationality, and gender; two critical care doctors; three patient representatives; 2 researchers, and 5–6 critical care educators are working collaboratively to co-design the guided reflective learning conversation model, in which clinical reasoning can be optimized with consideration to a wide range of case complexity, subspecialty, and competence levels. The co-design working group is meeting online for 4–6 workshops of 4 hours. The co-design process is built on valid and reliable clinical reasoning and educational theoretical frameworks and models. The inputs to the process, exercises, and activities are taking place during the workshops and the outputs of the workshops are described to establish the co-design process. The final draft of the model will be validated and tested. The study sample will be grouped into experimental and control cohorts of critical care nurses who attend critical care simulation-based courses (N=300). Data will be collected through surveys, focus groups, and simulation-based objective assessment and observations. The study has received Institutional Review Board approval from the Hamad Medical Corporation Medical Research Centre (MRC-01-22-117) and the University of Hertfordshire (HSK/PGR/UH/04728).
The first draft of the co-design model is presented in Figure 1. The final draft of the model will be released, validated, and tested in the near future using mixed methods research with comparative quasi-experimental and pre-test/post-test design.

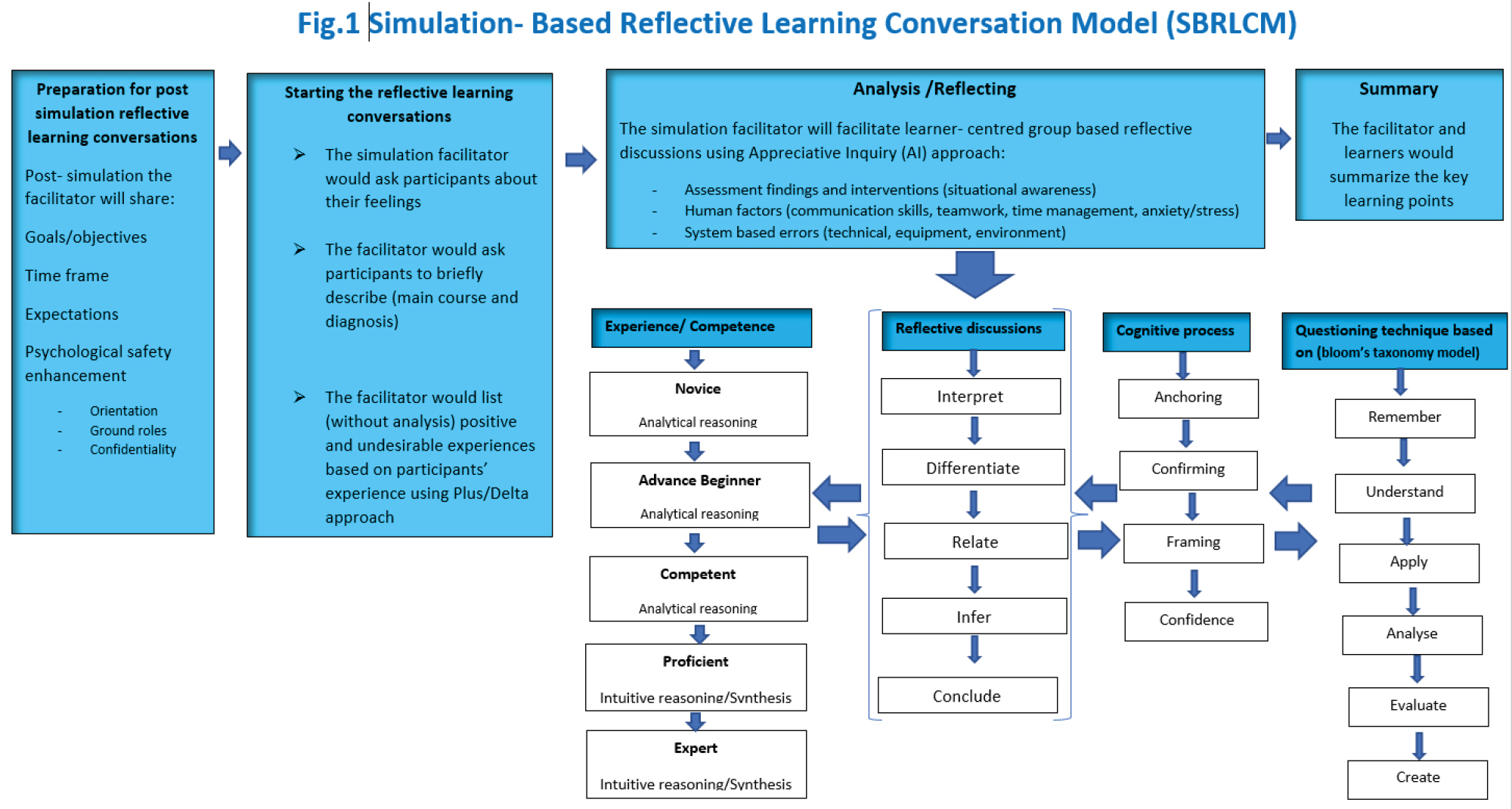
Clinical reasoning is multidimensional with difficulty to structure and evaluate during debriefing. Developing a guided reflective learning conversation model in which clinical reasoning skills are actively and effectively embedded, would therefore enable critical care nurses developing clinical reasoning skills to meet the special demands of critical care.
1. Vahedian-Azimi A, Hajiesmaeili M, Kangasniemi M, Fornés-Vives J, Hunsucker RL, Rahimibashar F, Pourhoseingholi MA, Farrokhvar L, Miller AC. Effects of stress on critical care nurses: a national cross-sectional study. Journal of intensive care medicine. 2019;34(4):311–22.
2. Kang H, Kang HY. The effects of simulation-based education on the clinical reasoning competence, clinical competence, and educational satisfaction. Journal of the Korea Academia-Industrial cooperation Society. 2020;21(8):107–14.
3. Decker S, Alinier G, Crawford SB, Gordon RM, Jenkins D, Wilson C. Healthcare Simulation Standards of Best PracticeTM The Debriefing Process. Clinical Simulation in Nursing. 2021;58:27–32.