
Corresponding author: Andrea Amato Gauci, [email protected]
” class=”pop” data-container=”body” data-toggle=”popover” data-placement=”bottom” href=”../../../search_author-andreaamatonullgauci”>Andrea Amato Gauci, ESRC Centre for Society and Mental Health, King’s College London, London, UK” class=”pop” data-container=”body” data-toggle=”popover” data-placement=”bottom” href=”../../../search_author-chrisnullattoe”>Chris Attoe, Institute of Psychiatry, Psychology & Neuroscience, King’s College London, London, UKESRC Centre for Society and Mental Health, King’s College London, London, UK
” class=”pop” data-container=”body” data-toggle=”popover” data-placement=”bottom” href=”../../../search_author-charlottenullwoodhead”>Charlotte Woodhead, Institute of Psychiatry, Psychology & Neuroscience, King’s College London, London, UKESRC Centre for Society and Mental Health, King’s College London, London, UK
” class=”pop” data-container=”body” data-toggle=”popover” data-placement=”bottom” href=”../../../search_author-stephanilnullhatch”>Stephani L Hatch, Faculty of Life Sciences and Medicine, King’s College London, London, UKSimulation and Interactive Learning Centre (SaIL), Guy’s and St Thomas’ NHS Foundation Trust, London, UK
” class=”pop” data-container=”body” data-toggle=”popover” data-placement=”bottom” href=”../../../search_author-ranjevnullkainth”>Ranjev Kainth
Previous research suggests that gender bias is pervasive in health care and has deleterious effects on treatment outcomes for patients. When developing and improving training on gender bias, we need to further our understanding of how such topics arise and are sustained in conversations between healthcare professionals (HCPs). The aim of this study is to analyze the influence of patient gender in HCP decision-making by analyzing how they surface, discuss and manage topics around gender.
An ethnomethodological qualitative study using discursive psychology and conversation analysis was implemented to examine 10 simulation debriefs in a specialized mental healthcare simulation centre in London. Video footage was obtained from mental health simulation training courses on bias in clinical decision-making, involving HCPs from mixed healthcare professions. Following transcription of selected segments, the debriefs were analyzed and repeated patterns of interaction were captured in distinct themes.
Four main themes were identified from the data, indicating some of the ways in which conversations about gender are managed: collaboration (to encourage discussion), surprise (when unexpected topics arose), laughter (to diffuse tense situations) and silence (demonstrating careful thinking). Patients with mental health conditions were perceived differently in terms of treatment decisions due to existing gender biases.
The persistence of gender bias that may result in discrimination in health care with negative consequences attests to the need for greater awareness and training development at various levels to include an intersectional approach.
What this study adds
• This study uses a novel approach to examine healthcare staff interactions through an ethnomethodological approach.
• It adds to existing research about discrimination within healthcare settings using simulation as a research tool.
• This study demonstrates the ways in which bias is co-created and given meaning within staff interactions and, in turn, affects perceptions and treatment of patients.
• Findings indicate potential avenues for improvements to current anti-discrimination training initiatives which incorporate awareness of how bias appears through language and non-verbal communication.
Discrimination continues to be an issue within health care globally, affecting both patients and staff [1–2]. For example, staff from minoritized groups with intersecting marginalized social statuses (a person’s social and political identities) within the National Health Service (NHS) are increasingly reporting discrimination to a greater extent than their White staff counterparts [1]. In relation to patients, research has consistently demonstrated that discrimination among marginalized groups can affect care, for example, acting as a barrier towards accessing healthcare services [3–4]. There is also evidence that discrimination affects the care offered to people, and that this may be manifested within interactions between staff and patients as well as between staff in clinical decision-making. In relation to race, evidence suggests that systematic differences in communication patterns between healthcare professionals (HCPs) and patients from marginalized and advantaged social statuses can impact patient care and decision-making through differential diagnoses [5].
Gender, also considering inclusively gender identity, continues to be one of the leading causes of discrimination [2]. Whilst discrimination is particularly evident for individuals occupying more than one disadvantaged social status, gender is one main category that impacts the care of patients with mental health illnesses with research attesting to the relationship between mental health and perceived gender discrimination [6]. Gender discrimination is pervasive across health care, for example, a review by Samulowitz et al. [7] found gender biases, in that male and female patients received differing treatment for chronic pain. In another study, African American women faced various stereotyping relating to their gender identity that presented barriers to accessing appropriate treatment care [8]. It is, therefore, understood that gender discrimination in health care across diverse settings has negative consequences on mental health and overall patient well-being.
Discrimination can be minimized through training around communication strategies involving interactions amongst HCPs [9]. However, few studies focus on patient perception of stigma and discrimination or long-term interventions in this area. The lack of research leads to increased miscommunication between patients and HCPs regarding treatment options [9]. As a result, it is unclear how topics of gender and gender bias are surfaced, discussed and managed between HCPs either in isolation or within an intersectional framework, and thus a void in knowledge exists. Before considering communication strategies in this field, it is thus critical to explore the question: how do HCPs discuss and manage topics around gender and gender bias?
One way to explore this gap is by examining verbal interactions between HCPs. Whilst there are other approaches to analyzing the construct of gender, we seek to examine how HCPs communicate gender-related issues during simulation debriefing where topics of gender and gender bias in relation to simulated exercises occur. This study specifically examines gender and gender bias in debriefing conversations in a mental healthcare simulation training setting undertaken at the Maudsley Hospital, which is the largest mental health training institution in the United Kingdom and has a dedicated research centre. It is part of the South London and Maudsley NHS Foundation Trust and works in partnership with the Institute of Psychiatry, Psychology & Neuroscience at King’s College London.
To understand the ways in which these topics are introduced and managed by participants through discourse, we must examine interactions directly. Ethnomethodology is an approach to understand how members (in this case, HCPs) undertake an activity, such as ‘managing discussions of gender’ [10]. The approach seeks to uncover the everyday ‘methods’ (such as conversational patterns and techniques) participants use within a culture to achieve the said activity. For example, a doctor–patient consultation (the activity) occurs through the roles which each participant takes, such as asking and answering questions, listing complaints and offering treatment options [11]. The analysis reveals patterns within conversations that form the interaction. Thus, the turns of talk have constructed the immediate social context – a typical doctor–patient consultation – and analysis of the discourse reveals the methods participants evoke to achieve the activity.
Within this methodological framework, conversation analysis (CA) is an approach that examines interactions in fine detail. Conversation analysts seek to elicit participants’ understanding of the ongoing conversational activity (comprised of what is being communicated and the ongoing interaction) by looking at subsequent turns of talk. Analysis of turns of talk will display, empirically, what the participant understood (or their display of understanding) regarding the previous turn, the ongoing activity that they are themselves co-constructing and the wider social context. CA is thus characterized by analyzing conversations between speakers and the meaningful impact these have in wider social practices [12] and in constructing the immediate context.
CA has been applied to explore interactions within institutional settings [13] and combined with the approach of discursive psychology (DP) in the empirical analysis [14,15]. DP is an approach that reveals how psychological themes manifest in conversations and the function of patterns in conversations. Moments of interactions can thus be observed in debriefs when HCPs discuss gender through a CA and DP lens, to analyze the discursive methods participants are involved in to achieve a social activity, namely the discussion of gender and gender bias.
CA has been researched for healthcare purposes such as in family therapy [16] and in medicine [17]. Additionally, CA and DP have been studied alongside each other in psychological research [18]. CA has also been used in research about educational institutions [19,20], which is pertinent, as the data analyzed were extracted from the simulation training centre at the Maudsley Hospital.
This study used existing videos from 10 debriefs ranging from 20 to 60 minutes taken from the simulation training centre at the Maudsley Hospital in South London, the first centre in the United Kingdom that focuses on mental health and the improvement of mental health services. The inclusion criteria consisted of participants taking part in a mental health simulation course on bias in clinical decision-making including discussions around social status. Participants consented to provide research data for the Maudsley Simulation team. Participants were aware that research would be conducted in different domains and would include the use of recorded data and transcripts. Ethics was granted by the King’s College London Psychiatry, Nursing and Midwifery Research Ethics Subcommittee on behalf of the Health Research Authority, PNM1314/173. This project was conducted as part of a postgraduate program in MSc Organisational Psychiatry & Psychology. None of the authors were faculty for this course. Furthermore, the first author is not a trained simulation debriefer. As such, the researchers had no contact and no direct influence with the participants. Segments of 10 out of 19 video recordings from 2015 to 2017 were intentionally selected, as these spoke about gender and thus were more likely to be of value to the research.
The participants in this study were HCPs, including doctors, nurses and healthcare assistants (Table 1). Patient case scenarios were portrayed by actors, trained to be simulated participants (SPs) with different social characteristics representing the South London population. For example, a male patient with psychosis was played by a black actor. All SPs underwent a two-day training course delivered by expert clinicians, patients and carers. This involved didactic teaching on educational theory; clinical presentations; patient testimonies, including recorded videos; and involvement in experiential simulations with feedback.
Furthermore, SPs were treated as part of the training team, joining morning, lunch and post-course briefings, as well as observing debriefs alongside technicians to help support the learning of participants. The course lead (a trained clinician) would communicate with the SPs throughout and at the end of the day to monitor their experiences and state of mind, and to provide feedback on their role in the training. Participants’ feedback on the actors was also sought and shared as another stream of information to refine their performance. The intention of such extensive training and continual feedback was to enable accurate patient portrayal, including encouragement to be responsive to the ongoing interactions with the HCPs, which maximized psychological fidelity for HCPs.

| Year (n = number of debriefs) |
Healthcare Professions |
|---|---|
| 2015 n = 6 |
Registered mental nurses (RMNs) = 4 Psychiatry trainees = 4 |
| 2016 n = 7 |
RMNs = 5 Social workers = 2 General practitioner = 1 Psychiatry trainees = 4 |
| 2017 n = 6 |
Psychiatry trainees = 2 Social workers = 2 RMNs = 6 Occupational therapists = 2 |
The Making the Challenging Clinical Decision course included a diverse mix of healthcare professions, and the data presented here are representative of the course that ran over 3 years.

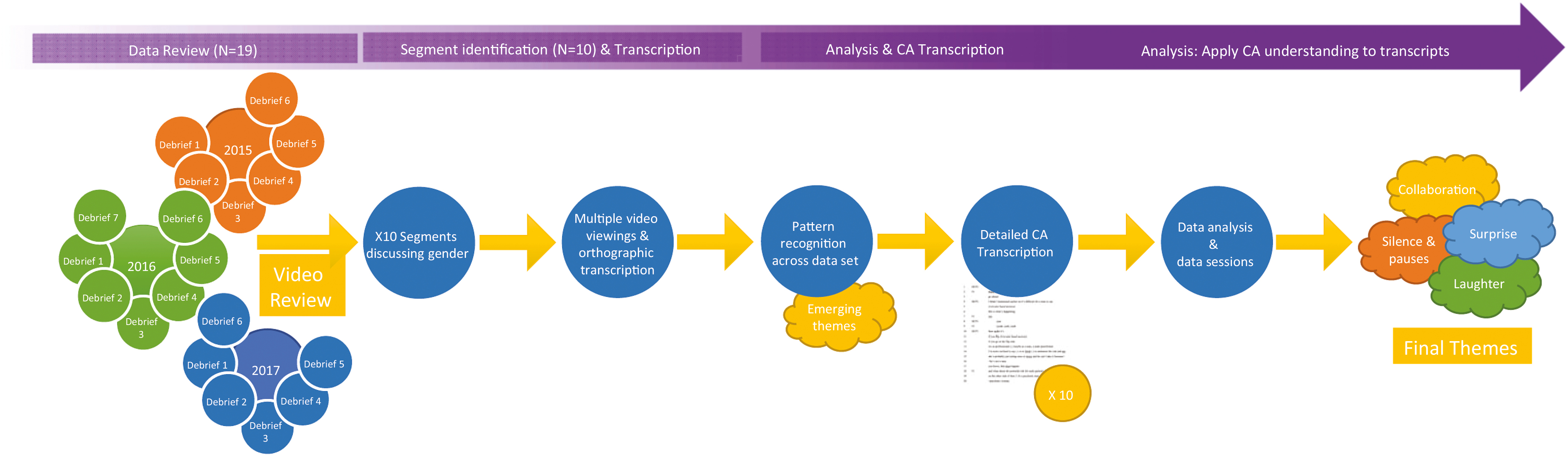
Phases of data collection and analysis for this study
Each of the 10 debriefs was reviewed, and segments, where gender as a topic was discussed, were identified. Each video recording and segment was then transcribed using a modified Jeffersonian system adapted from Wetherell et al. [21] (Table 2). This included fine detail including pauses, intonation and pitch depending on interactional relevance and in sufficient detail to allow analysis through a DP lens. Details including non-verbal gestures were deemed relevant as speech alone does not fully capture all modes of communication. Each segment was analyzed for reoccurring patterns, which were then used to observe how these patterns were created turn by turn.

| Symbol | Description |
|---|---|
| [yes | Words enclosed with a left square bracket indicated overlapping talk |
| = | Ongoing speech between lines or there were no gaps/pauses in between lines in transcript |
| (.) | A pause in conversation less than a second long |
| (1.0) | Time (in seconds) between the end of a word and the start of the next word |
| Yes | Underlining words indicated speaker emphasis |
| ↑↓ | An upward arrow indicated marked raise in speaker intonation, whereas a downward arrow indicated decreased intonation |
| ((description)) | Double parentheses indicated descriptions that reflected the speaker’s non-verbal actions |
The participants were anonymized during transcribing with the labels ‘HCP’ and numbered according to how many HCPs spoke during the debrief session (e.g. HCP1 and HCP2). The facilitators of the sessions were anonymized with the label ‘F’ (for facilitator) and similarly numbered.
Four main themes were identified in this study as CA was applied to conversations held between HCPs and faculty in decision-making for mental health patients of differing social statuses. Analysis revealed the need for collaboration, displayed as interactional encouragement, to discuss gender bias as the main topic of conversation. HCPs display surprise, when HCPs delay conversing about domestic violence that occurred by a female patient. For laughter, HCPs fail to acknowledge the differences between male and female patients with psychoses, and this facilitates a cushioning effect in an uncomfortable interaction. Silence and pauses presented as hesitation when HCPs describe a male patient with psychosis as impulsive and violent, demonstrating consideration before discussing a potentially controversial statement. The themes of surprise and laughter reveal how sensitive issues can create uncomfortable interactions between HCPs. The theme silence and pauses demonstrates the cautious approach taken to discuss sensitive issues, particularly related to patient gender and domestic violence.
The theme ‘collaboration’ displayed how multiple individuals can purposefully encourage other participants to construct the topic of discussion, often centred around gender bias. The following is an extract from a debrief session occurring in 2017 and follows a conversation between a facilitator (F1) and one HCP (HCP1). Before this extract, the facilitator discussed with the HCPs the differences in treatment decision-making for two patients with psychoses. In particular, F1 questioned why the HCPs appear to be more concerned about the outcome of the male than the female patient with psychosis:

| 1 | HCP1 | I think there’s, there’s gender bias= =isn’t there |
| 2 | F1 | thank ↑ you for bringing that up |
| 3 | go ahead | |
| 4 | HCP1 | I think I mentioned earlier on it’s= =difficult for a man to say |
| 5 | ((circular hand motion)) | |
| 6 | this is what’s happening | |
| 7 | F1 | yes |
| 8 | HCP1 | [um |
| 9 | F1 | [yeah, yeah, yeah |
| 10 | HCP1 | then again it’s |
| 11 | if you flip ((circular hand motion)) | |
| 12 | if you go in the flip side | |
| 13 | we as professionals (.) maybe as a= =man, a male practitioner |
|
| 14 | I’m more inclined to say (.) or= =to think (.) to minimize the risk= =and say |
|
| 15 | she’s probably just acting once or= =twice and he can’t take it because= |
|
| 16 | =he’s not a man | |
| 17 | you know, that does happen | |
| 18 | F1 | and what about the potential risk= = for male patients then? |
| 19 | on the other side of that (1.0) a psy= =chotic man is a lot scarier than a= |
|
| 20 | =psychotic woman |
In extract one , F1 responded to HCP1 when the topic of gender bias arose. The rise in intonation indicates the emphasis portrayed by F1, demonstrating a want for this conversation. The words ‘thank you’ (L2) also show appreciation and acknowledgement for the participant to continue the conversation. F1 requested further elaboration from HCP1 (L3, L7 and L9), and HCP1 collaborated with F1 by progressing the interaction, responding to their encouragement. F1 used this interaction to make a final point in highlighting the influence of gender on psychosis (L18–20). This extract, therefore, resonates with Weingarten [22] in that meaningful discussions are extended, and this encourages the management of conversation flow [23]. Albeit the extent of collaboration in conversations differs [24], this extract provides a good example of the use of certain utterances (‘yes’, ‘yeah’) to re-enforce further discussion in an ongoing interaction. In this way, collaboration through these mechanisms allows for gender bias to be constructed as a valid topic of conversation.
Extract one displays the need for discursively constructing vindication to allow discussions on gender which subsequently influences HCP decision-making. Another example of collaboration occurs through the use of certain utterances in extract three where HCP1 and HCP2 responded to the facilitator’s questions by repeating ‘mhm’ (L2 and L4). In this way, collaboration materializes through turn-taking in conversation via a series of questions and answers.
In this study, the theme surprise demonstrated resolution to unmet expectations for certain topics. Extract two is from a debrief session in 2017. Two facilitators (F1 and F2) presented the HCPs with a task to list points for or against discharging a female patient. Before this conversation, the HCPs established a history of domestic assault on the patient’s husband, caused by the patient:

| 1 | F1 | anything to do with the family (.)= =to start? |
| 2 | F2 | negatives for discharge, I don’t= =understand why that box is empty |
| 3 | I’m confused ((playing with own hair)) (2.0) | |
| 4 | F1 | negatives for discharge (2.0) |
| 5 | HCP1 | but also (.) she might be the im= =pact on the children (.) |
| 6 | like if she’s um (.) like hitting the= =husband |
|
| 7 | that will be affecting the children [the stress | |
| 8 | F2 | [yeah ↑ |
| 9 | she’s hitting ↑ the husband | |
| 10 | F1 | ((writing on a flip board)) |
| 11 | HCP2 | we can actually say that (6.0) |
| 12 | HCP1 | and the impact on the husband as= =well ((sigh of laughter)) |
In extract two , F2 presents surprise when HCP1 stated that the patient can cause harm to her family if she returns home as she has a previous history of assaulting her husband, which will have negative consequences on their children (L5–7). F2 displayed surprise in L2 and L9 in different ways. In L2, F2 revealed surprise that nobody brought up the patient’s history of abuse on her husband. This is constructed discursively using the word ‘confused’ and embodied by ‘playing with own hair’. The function is to demonstrate to participants that there may be a reason for the surprise and thus forces them to consider alternative options which were not considered (e.g. hitting the husband). In L9, this surprise is more apparent as F2 immediately responded to HCP1. As a result of this surprised response, another HCP (HCP 2) stated ‘we can actually say that’ as now the topic is out in the open: it has been discursively constructed. HCP1 acknowledged F2’s surprise with a sigh of laughter. For this extract, surprise resonates with the literature in that F2 responded without delay [25] to L7 and, in fact, interrupted HCP1 from elaborating further (L8). Contrary to Wilkinson and Kitzinger [26] where surprise is a result of unexpected talk, F2 is surprised that the topic of domestic violence is delayed. Agreeing with Wilkinson and Kitzinger [26], however, surprise in this extract appears repetitive (L9 is a repeat of L6) and serves to validate the participant’s response.
Additionally, in this extract, a female patient is seen as less able to cause harm to her family despite a violent history. Gender, in this case, influences HCP decision-making in that a female patient with a history of violence is less likely to be admitted in an inpatient ward and, therefore, is more likely to be re-united with her family. F2 is constructing surprise and the way they are doing so is by emphasis, change of tone and overlap of conversation (L8 and 9). Surprise is constructed as the gender of the patient should not be the main reason whether this patient is capable of committing domestic violence, but her history of violence should. In this way, surprise is used as a social action to demonstrate that the group has demonstrated gender bias.
The theme laughter presented when HCPs met with uncomfortable interactions and functioned to reduce tension. Like extract one, the following extract presents the same context in observing the differences between how HCPs treat male and female patients with psychoses. This session was in 2015 and, therefore, represents a different cohort of HCPs than the 2017 session. One facilitator and three HCPs featured in extract three. The facilitator addressed the patients with psychoses and compared them to begin the discussion:

| 1 | F1 | this is our second psychotic per= =son of the day right? |
| 2 | HCP1 | mhm |
| 3 | F1 | do you guys remember our psy= =chotic person from the morning? |
| 4 | HCP2 | mmhm |
| 5 | F1 | I just don’t |
| 6 | I’m a little curious about the dif= =ference in feelings about our two |
|
| 7 | psychotic patients (3.0) | |
| 8 | the fears this morning don’t seem= =to be (1.0) appearing this afternoon |
|
| 9 | but they’re two psychotics, I, I= | |
| 10 | =I just don’t understand | |
| 11 | HCP2 | different variables attached to= =both |
| 12 | F1 | what are those variables? |
| 13 | HCP2 | quite a few, quite a lot |
| 14 | F1 | go ahead |
| 15 | HCP2 | oh, goodness |
| 16 | ((several people laughing)) | |
| 17 | HCP3 | people can help you out |
| 18 | HCP2 | yeah please do |
| 19 | umm (3.0) no | |
| 20 | sorry (.) sorry | |
| 21 | F1 | okay that’s fine (.) that’s fine |
| 22 | anybody? | |
| 23 | HCP4 | I guess the risk profile (.) um,= =single (.) male (.) umm (.) young= =ish, um |
| 24 | I don’t know what her age was= =again |
Extract three portrays the effect laughter has when HCP2 is confronted with F1 to elaborate on the ‘different variables’ attached to the female patient with psychosis. HCP2 did not prepare a response and replies with ‘oh, goodness’ (L15). Several HCPs laughed during the session until HCP3 suggested that other HCPs can assist HCP2; however, this assistance does not occur until later in the conversation (L23). Before this assistance, HCP2 struggled to provide a response to F1, who progresses the dialogue. In this extract, laughter serves to manage an uncomfortable interaction [27], specifically to manage and ensure the conversation can continue to reach a topic of gender bias as HCP2 fails to sufficiently respond to F1. Furthermore, L15 demonstrates a rejection to a problematic situation [28] by not responding adequately. However, this works more to reduce the tension than avoid the topic altogether [29]. The latter is true as although HCP2 did not elaborate, they did make an attempt to and did not discard the topic (L18–20).
The above extract pertains to the difficulty in discussing patient gender differences when patients have similar diagnoses. Gender as a factor is not easily surfaced, and laughter is used to mitigate for not being able to find appropriate determinants. This difficulty is explicit through laughter, and HCP3 recognized this and manages the interaction by lessening the pressure for one HCP to respond to F1 (L17). To rectify the situation, HCP4 resorted to other clinical evaluation methods to discuss patient differences, namely the differences in risk profiles (L23-24). The frequency of pauses (L23) included when discussing risk profiles reflects careful decision-making [29] constructed as a three-part list as HCP4 led a new topic of conversation. Laughter may indicate trouble in participants analyzing or understanding the role of determinants and how HCPs make decisions accordingly.
Whilst silence and pauses elicit many meanings in the literature [30], this paper revealed a cautious functionality for this theme in that HCPs carefully thought out their decisions as individuals with the authority to alter the course of treatment for mental health patients. The fourth and final extract for this chapter was from a session in 2016. One facilitator interacted with four HCPs in discussing a male patient, particularly over concerns that he is violent. Before this extract, HCP4 is engaged in conversing about this patient and later refers to this engagement in L14:

| 1 | HCP1 | ↓that he’s impulsive somewhere? |
| 2 | F1 | impulsive? |
| 3 | HCP1 | did I hear that?= |
| 4 | F1 | =did I hear what |
| 5 | HCP1 | that he was impulsive somewhere |
| 6 | was it? | |
| 7 | impulsive nature | |
| 8 | F1 | impulsive |
| 9 | HCP2 | well he mentioned it= |
| 10 | HCP1 | =it came up |
| 11 | F1 | impulsive in what way though |
| 12 | HCP3 | we’re talking about behaviours in= =terms of right in front of us |
| 13 | I think he mentioned it very clearly | |
| 14 | HCP4 | he may not do it, my point is I’m= =not talking about him per se |
| 15 | but what I am saying is sometimes= =(.) people make non-violent |
|
| 16 | they don’t perceive something to= =be violent, but the outcome will be |
|
| 17 | violent, you said to me= | |
| 18 | =that he was a non-violent per-= =son but |
|
| 19 | F1 | sure |
| 20 | yeah | |
| 21 | HCP4 | actually decisions made (1.0) can= =still result in harm= |
| 22 | F1 | okay |
| 23 | HCP4 | =in that’s, that’s |
| 24 | F1 | sure, sure |
| 25 | but the only impulsive thing we’ve= =seen him doing is just being= |
|
| 26 | =really obnoxious and annoying= =about (.) wanting to spread the word= |
|
| 27 | =of, of Buddhism (.) of enlighten-= =ment |
In extract four, silence is portrayed as a series of pauses and hesitancy during a conversation where a male patient is impulsive and, therefore, potentially violent. HCP1 was hesitant to question whether the patient was impulsive (L1), and this is reflected through lowering the intonation. This lower intonation is received by F1, who clarified whether they had heard HCP1 correctly (described in CA as repair). Later in the interaction, HCP4 paused before stating that the said patient is indeed violent (L15) and reiterated this after pausing once more (L21). Finally, F1 clarified that there is no evidence to suggest that the patient is violent, rather he wanted to ‘spread the word of Buddhism’ (L26 and 27).
Furthermore, the lower intonation from HCP1 suggests the lack of knowledge of whether the patient is impulsive, and this resonates with Berger [30] on uncertain speech. HCP4 paused a few times before stating that the patient is probably violent, and this resonates with Ephratt [31] in demonstrating careful decision-making before conversing. In this way, HCP4 carefully constructed their statements before making an explicit point that this patient is violent. This caution is understandable considering an HCP has to be mindful before announcing such a serious accusation about a mental health patient.
Additionally, silence is portrayed in extract one when HCP1 delivered their message on gender bias with the use of gestures (L5 and L11), and this echoes the work by Al Jahdhami [32] in the use of non-verbal communication to elicit meaning. Similar to extract four, in extract one , HCP1 paused a few times before elaborating on gender bias (L13 and 14), and this indicates thoughtful conversation [31]. Silence is also exhibited in extract two, where HCP2 validated the domestic abuse that occurred within a patient’s family (L12), and after 6 seconds, this is confirmed through acknowledgement of HCP1 (L13). The function of silence and pauses here is that HCP2 has stated an opinion of position (L12).
The influence of gender in extract four pertains to the stereotype that male patients with psychoses are more impulsive and thus more likely to cause violence. Furthermore, this male patient explicitly stated that he does not believe in violence. This finding is relevant to compare with extract two where a female patient who does have a history of violence is not taken as seriously. In this way, HCP decision-making is influenced by patient gender in that there is more caution for male patients with psychoses and the ability to cause harm, whereas the opposite is true for female patients with psychoses. The analysis shows that HCPs must use a range of discursive devices to surface gender bias relating to a female patient in comparison to a male patient with psychosis.
The aim of this study was to analyze the influence of patient gender in HCP decision-making and address the gap in research in this area. Specifically, we sought to understand how HCPs discuss and manage topics around gender as this may influence future research and training interventions. A detailed analysis of the transcripts revealed four themes (collaboration, surprise, laughter and silence and pauses). The patterns of talk observed in this study demonstrate the sensitive way in which gender and gender bias are discussed by HCPs.
There is evidence of gender bias and disparities within health care [33], including gender stereotyping for patients [34]. In this study, the topic of gender bias required encouragement from someone acting as a ‘facilitator’ within the interaction as featured in the collaboration theme. Although it did take time for an HCP to present the topic of gender bias, once raised, the facilitator collaborated with the HCP to discuss this as it applied to a female patient with psychosis. The reinforcement provided by the facilitator worked to progress the discursive construction of gender bias, which was critical, as avoidance of this topic creates resistance for patients to receive accurate diagnosis and treatment [35]. Despite the sensitivity in discussing gender bias due to social desirability, the results of this study revealed an outward and open conversation which was unexpected. The collaboration theme, therefore, facilitated the acknowledgement of patient gender in HCP decision-making and was an important conversation to be had before deducing treatment options.
Furthermore, gender discrimination within health care tends to arise from stereotypes applied to male and female patients, where men are expected to suffer more from alcohol and substance abuse, and women from ‘emotional’ conditions [34]. The analysis of the surprise theme presents the disbelief in the possibility of a female patient committing domestic violence. A comparison between a male and a female patient with psychoses appears once more in the silence and pauses theme. The results show the disparity in perceptions that a female patient with psychosis is less likely to perpetrate domestic violence than a male patient with psychosis. The male patient is further described as ‘impulsive’ by HCPs despite the facilitator disregarding this comment due to his belief in non-violence, and the participant responds to this with repair to soften the statement. This generalizing outlook on male patients appearing more violent could lead to further reduced healthcare quality [5], and discrimination in mental health conditions has been shown to have negative consequences that supersede physical health issues [4,7]. The reinforcement of a negative social stigma, such as gender stereotyping, may also lead to avoidance for these patients in accessing clinical care [35]. In this way, HCP decision-making that re-enforces such stereotypes may neglect critical treatment care and overall quality of care for these patients.
Increasing awareness of how gender biases arise within healthcare interactions and how biases influence individual decision-making and treatment outcome would be a potentially valuable avenue to enhance existing formal professional training interventions or programmes. Training can increase awareness of multiple social cues, as indicated in CA, as both what is said and how it is said can create the immediate social context around gender bias.
Presently in the United Kingdom, HCPs, such as nurses and psychiatrists, and other professionals are required to revalidate their licences after some years to ensure their ability to practice their professions by applying the latest evidence-based procedures and treatment strategies are maintained. Continuing medical education is another important element for HCPs to effectively practice and develop within their professions with different means of training (e.g. analyzing clinical cases [36]). Both programmes should include an emphasis on the manifestations and impact of gender bias in patients from a disadvantaged background on their clinical decision processes.
Specifically, training can raise awareness of these persisting issues to create a more positive, and collaborative working environment between HCP and patients. CA allowed for an in-depth analysis of sensitive topics that are not always explicitly discussed, and DP inferred these psychological domains from a wider societal perspective, particularly within healthcare communities. Training is an opportunity to examine sensitive, intersectional areas such as gender bias which notoriously are difficult areas of discussion.
While this study focussed on gender, research illustrating the importance of intersectionality suggests that formal training of HCPs should also include consideration of multiple social statuses in exploring patient experiences so that such training is more inclusive and representative. Healthcare educators can encourage more dialogue to discuss sensitive topics that impact patient experiences. Such skills development can be included in continuing medical education practices and re-validation as part of improving healthcare outcomes for individuals from intersectional social statuses. HCPs able to discuss biases and sensitive issues in an educational setting create a safe space to raise such concerns and learn how to address them alongside the assistance of healthcare educators. Integrating such activities will allow for a field willing to evolve and account for these issues.
The findings of this study suggest that gender bias is still prevalent amongst HCPs, and thus gender discrimination persists amongst mental health patients. Data were analyzed in relation to male and female dichotomy between 2015 and 2017. It is important to recognize that gender identity is no longer considered to be dichotomous leaving opportunities to conduct further research exploring this area. Albeit the findings in this paper present gender as the main discriminatory factor, these other intersecting social categories contribute to the patient’s unique experiences [37], and, therefore, the impact of discrimination is likely to be more complex than reported here.
As with all ethnomethodological work, there are limitations in terms of data recordings. Specifically, video recordings will capture certain angles of interaction and can thus never be considered neutral. It may not always be possible to hear everything from participants or see everyone’s eye gaze movement. Transcriptions are based purely on what can be heard and the level of transcription provided here is done so on the basis to achieve the research aims, although traditional conversation analysts may argue that finely detailed transcription may reveal additional findings.
The themes in this study highlight the patterns of talk which occur when there are discussions around patient gender, and there is evidence within these extracts that patient gender can influence HCP decision-making. Perceptions of female and male patients with mental health conditions differed in terms of treatment outcomes, and gender biases persisted for both patients over the course of the debriefs. The persistence of gender bias and thus discrimination in health care attests to the need for developments in training, as people do have intersecting social statuses which makes it important that these findings are explored and expanded to appraise how bias is surfaced in relation to those multiple statuses.
AAG is the primary author and undertook this project as part of a postgraduate program, MSc Organisational Psychiatry & Psychology, at King’s College London. AAG undertook transcription and data analysis. RK is the senior author and provided support on methodology and methods and undertook joint data sessions with AAG. CA, SLH, and CW were involved in supervising AAG. All authors contributed to the review and editing of the final manuscript.
SLH is part-funded by the NIHR Biomedical Research Centre at South London and Maudsley NHS Foundation Trust. CW and SLH are supported by the ESRC Centre for Society and Mental Health at King’s College London (ESRC Reference: ES/S012567/1). The funders had no involvement in study design, data collection, analysis, interpretation or the decision to submit for publication. The views expressed are those of the authors and not necessarily those of the funders.
None.
None declared.
The authors declare that they have no conflict of interest.
1.
2.
3.
4.
5.
6.
7.
8.
9.
10.
11.
12.
13.
14.
15.
16.
17.
18.
19.
20.
21.
22.
23.
24.
25.
26.
27.
28.
29.
30.
31.
32.
33.
34.
35.
36.
37.