
Virtual reality (VR) is an expanding area within medical education, accelerated by the COVID-19 pandemic. Use of VR has been explored within multiple areas but there is limited evidence relating its use in teaching clinical decision-making (medical ‘expert-thinking’) to medical students [1]. Before VR, the most realistic patient-less simulation environments utilised high-fidelity manikins (HFSim). These are effective in teaching management of numerous medical and surgical presentations, but limited by cost and logistics [2]. This is the first study to assess the efficacy of VR, compared to HFSim, in teaching medical students’ clinical decision-making.
This ethically approved study utilised mixed methods to investigate:
Whether VR is as effective as HFSim at increasing students’ clinical decision-making competence and confidence;
The perceived value and experience of each; and
Where VR training should be placed temporally in relation to HFSim.
Sub-analyses explored whether outcomes were influenced by gender.
Students were randomly allocated to experience a simulated scenario in either VR or HFSim. After consenting, participants:
1. Completed baseline assessments of competence and confidence;
2. Received sepsis revision and familiarisation with the relevant environment;
3. Individually undertook an acute sepsis scenario with debriefing;
4. Completed follow-up confidence and competence assessments;
5. Undertook a second scenario in the alternate environment; and
6. Completed questionnaires regarding experiences of VR and HFSim, and preferred initial environment.
The collated data was analysed using the t-test in Excel®.
The study recruited 50 participants. Key findings were:
1. No difference in baseline confidence between VR and HFSim groups;
2. Statistically equal increase in confidence and competence regarding decision-making (confidence after VR +17% and HFSsim +19%, competence after VR +17% and HFSsim +15%). See Figure 1;

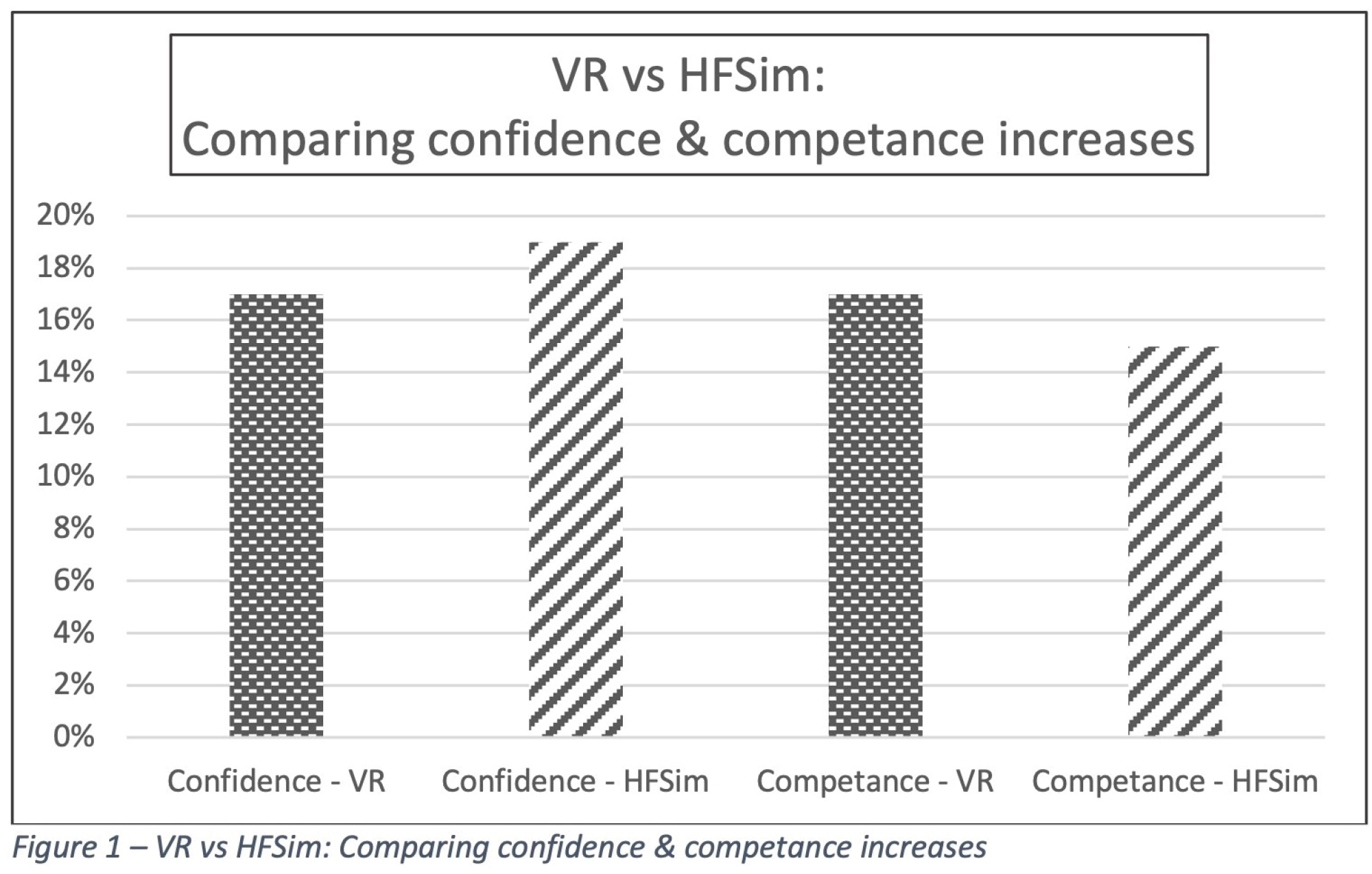
3. Participants’ preference was for HFSim (71%, due to greater realism; increased pressure; and verbal communication);
4. Participants’ preference was to undertake VR before HFSim (80%, because less stressful and useful earlier in training); and
5. 100% recommended both environments (complement each other and different knowledge gained from each).
Sub-analysis revealed same outcomes with gender aggregation.
Interim results suggest, regardless of gender, equivalent increases in confidence and competence are achieved in teaching clinical decision-making with either VR or HFSim. VR appears to have a natural place in the progression of teaching between theory and HFSim. Evidence suggests that teaching ‘expert-thinking’ should begin early in training [3]. VR simulation is a safe and more moderate technique through which this can be introduced.
1. Jiang H, Vimalesvaran S, Wang JK, Lim KB, Mogali SR and Car LT. Virtual Reality in Medical Students’ Education: Scoping Review. JMIR Med Educ. 2022; 8(1):e34860.
2. Haerling KA. Cost-utility analysis of virtual and mannequin-based simulation. Simul Healthc. 2018;13(1): 33–40.
3. Garfield J, Le L, Zieffler A and Ben-Zvi D. Developing students’ reasoning about samples and sampling variability as a path to expert statistical thinking. Educ Stud Math. 2015; 88(3): 327–342.